Traumatic injuries involving the spine are treated as medical emergencies because of the vital role the spinal column plays in protecting the spinal cord and supporting movement. Whether trauma results from a motor vehicle collision, fall, sports injury, or other sudden impact, emergency room teams follow a structured process to identify potential spinal damage quickly and safely. Comprehensive Spine Care in New Jersey often educates patients on what happens during emergency spine evaluations so they can better understand how decisions are made during these critical moments. Knowing how spine trauma is assessed can help clarify why certain tests are performed and why precautions are taken even when symptoms are not immediately severe.
Why Spine Injuries Require Immediate Evaluation
The spine serves as both a protective structure for the spinal cord and a flexible framework that allows movement. Trauma can disrupt this balance, potentially affecting bones, discs, ligaments, nerves, or the spinal cord itself. Because spinal cord injuries may result in permanent neurological deficits, emergency teams treat suspected spine trauma with caution from the moment a patient arrives.
Symptoms of spinal injury are not always immediately obvious. Some individuals may walk into the emergency room with minimal pain, while others experience delayed neurological changes hours after the injury. For this reason, emergency protocols assume a possible spine injury until proven otherwise. Stabilization and careful evaluation help reduce the risk of worsening an undetected injury.
Spine trauma assessments are designed to identify both obvious and subtle injuries. Even low-energy incidents, such as a fall from standing height in older adults, can result in fractures or instability, particularly in individuals with underlying bone or degenerative conditions.
Initial Stabilization and Triage in the ER
When a patient arrives at the emergency room after trauma, the first priority is stabilization. Emergency medical personnel often immobilize the spine before arrival using a cervical collar and backboard. This precaution limits movement until spinal injury can be ruled out.
During triage, clinicians assess vital signs, level of consciousness, and the mechanism of injury. High-impact mechanisms such as car accidents or falls from height raise suspicion for spinal trauma. Patients are asked about pain, numbness, weakness, or difficulty moving their limbs.
If a patient is unconscious, confused, or unable to communicate clearly, clinicians rely heavily on physical findings and imaging. In these cases, spinal precautions are maintained until thorough evaluation confirms that it is safe to remove immobilization devices.
Neurological Examination and Physical Assessment
A detailed neurological exam is a key component of spine trauma evaluation. Clinicians assess motor strength, sensation, reflexes, and coordination in the arms and legs. These findings help determine whether the spinal cord or nerve roots may be affected.
The physical exam also includes careful palpation of the spine to check for tenderness, deformity, or step-offs that may indicate fracture or dislocation. However, the absence of pain does not rule out injury, especially in patients with altered mental status or distracting injuries.
Neurological findings guide urgency and next steps. Weakness, numbness, loss of sensation, or bowel and bladder changes raise concern for spinal cord involvement and often prompt immediate advanced imaging and specialist consultation.
Imaging Studies Used in Spine Trauma Evaluation
Imaging plays a central role in evaluating spinal injuries. The choice of imaging depends on the location of suspected injury, the severity of trauma, and clinical findings.
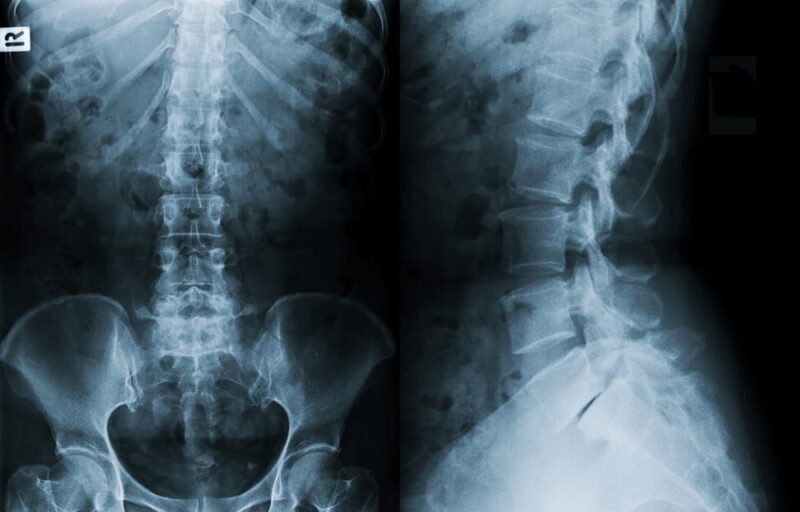
X-rays may be used in some cases to assess alignment and detect obvious fractures, but they are limited in their ability to visualize complex injuries. Computed tomography (CT) scans are commonly used in emergency settings because they provide detailed images of spinal bones and can quickly identify fractures or dislocations.
Magnetic resonance imaging (MRI) is particularly useful for evaluating soft tissues, including discs, ligaments, spinal cord, and nerve roots. MRI may be ordered when neurological symptoms are present or when ligamentous injury is suspected despite normal CT findings. These imaging tools work together to provide a complete picture of spinal integrity.
Identifying Different Types of Spine Trauma
Spine trauma can involve a wide range of injuries, from minor compression fractures to severe spinal cord damage. Common categories include fractures, dislocations, disc injuries, and ligamentous instability.
Compression fractures are often seen in the thoracic or lumbar spine and may result from axial loading forces. Burst fractures involve multiple fracture fragments and may compromise the spinal canal. Dislocations occur when vertebrae shift out of alignment, often causing instability.
Soft tissue injuries, such as torn ligaments or herniated discs, may not be immediately visible on basic imaging but can still result in pain or neurological symptoms. Conditions such as spine trauma and fractures encompass a wide spectrum of injury severity, which is why thorough evaluation is essential.
Role of Spine Specialists in the Emergency Setting
When significant spine trauma is identified or suspected, emergency physicians often involve spine specialists such as orthopedic spine surgeons or neurosurgeons. These specialists review imaging, assess neurological findings, and help determine whether surgical or non-surgical management may be considered.
Specialist input is particularly important in cases involving spinal instability, spinal cord compression, or progressive neurological deficits. Collaboration between emergency physicians, radiologists, and spine specialists ensures that care decisions are based on a comprehensive understanding of the injury.
Not all spine injuries require surgery. Many stable fractures and soft tissue injuries are managed with bracing, activity modification, and close follow-up. Determining stability is a key outcome of the emergency evaluation process.
Monitoring and Ongoing Assessment
Spine trauma evaluation does not end with initial imaging. Patients may be observed in the emergency department or admitted to the hospital for ongoing monitoring. Neurological status is reassessed regularly to detect any changes that may indicate evolving injury.
Pain management, supportive care, and prevention of complications are addressed during this phase. In some cases, repeat imaging may be necessary if symptoms change or if initial studies are inconclusive.
Patients with minor injuries may be discharged with instructions for follow-up evaluation, while those with more serious injuries may require inpatient care or transfer to a trauma center.
Why Some Spine Injuries Are Difficult to Detect
Certain spinal injuries can be subtle, especially in the early stages. Ligament injuries, small fractures, or disc-related trauma may not cause immediate symptoms. Adrenaline and shock can also mask pain shortly after injury.
Delayed symptoms such as increasing pain, stiffness, numbness, or weakness may emerge hours or days later. This is why emergency clinicians take conservative precautions and rely on imaging rather than symptoms alone when evaluating potential spine trauma.
Understanding that spine injuries may evolve helps explain why patients are advised to seek evaluation after trauma, even if they initially feel well.
What Patients Can Expect After ER Evaluation
After spine trauma evaluation, patients are informed about imaging results and next steps. This may include discharge instructions, referrals for follow-up care, or admission for further treatment. Education is an important part of this process, helping patients understand activity restrictions, warning signs, and recovery expectations.
Patients are often advised to avoid certain movements, wear braces if prescribed, and seek prompt care if neurological symptoms develop. Clear communication helps ensure safety after leaving the emergency setting.
Emergency Spine Trauma Assessment
Spine trauma evaluation in the emergency room follows a structured and cautious process designed to protect neurological function and identify injuries accurately. From stabilization and neurological exams to advanced imaging and specialist consultation, each step plays a role in ensuring patient safety.
Understanding what happens during emergency spine trauma evaluation can help patients feel more informed during a stressful experience. Comprehensive Spine Care in New Jersey emphasizes education to help individuals better understand how spinal injuries are assessed and why careful evaluation is essential after traumatic events.
Sources
Vaccaro, A. R., et al. (2013). Spine trauma: Diagnosis and management. The Journal of Bone and Joint Surgery.
Daffner, R. H., & Weissman, B. N. (2007). Imaging of spine trauma. Seminars in Roentgenology.
American College of Surgeons Committee on Trauma. (2018). Advanced Trauma Life Support (ATLS) Student Course Manual.