Headaches are a common ailment that affects millions of people worldwide. While they can be caused by various factors, one often overlooked source is neck pain. The intricate relationship between the neck and headaches is often misunderstood, leading individuals to treat the symptoms without addressing the root cause. In this blog, we will delve into the connection between headaches and neck pain, explore the possible reasons behind this link, and shed light on the available treatments provided by spinal specialists.
Understanding the Link between Headaches and Neck Pain
The relationship between headaches and neck pain is complex and often interconnected. Headaches can be caused or exacerbated by issues originating in the neck, and conversely, neck pain can sometimes be a result of headaches. This connection is known as cervicogenic headaches.
Cervicogenic headaches are a specific type of headache that originates from problems in the cervical spine (neck). The pain typically starts in the neck and then radiates to the head, causing headaches. This type of headache can be challenging to diagnose, as the pain is often referred from the neck to the head, and individuals may not always associate their headaches with neck issues.
Cervicogenic headaches can be caused by:
- Shared Nerve Pathways: The neck and the head have shared nerve pathways, which means that pain signals can be transmitted between these regions. Irritation or compression of nerves in the neck can lead to pain signals being transmitted to the head, resulting in headaches.
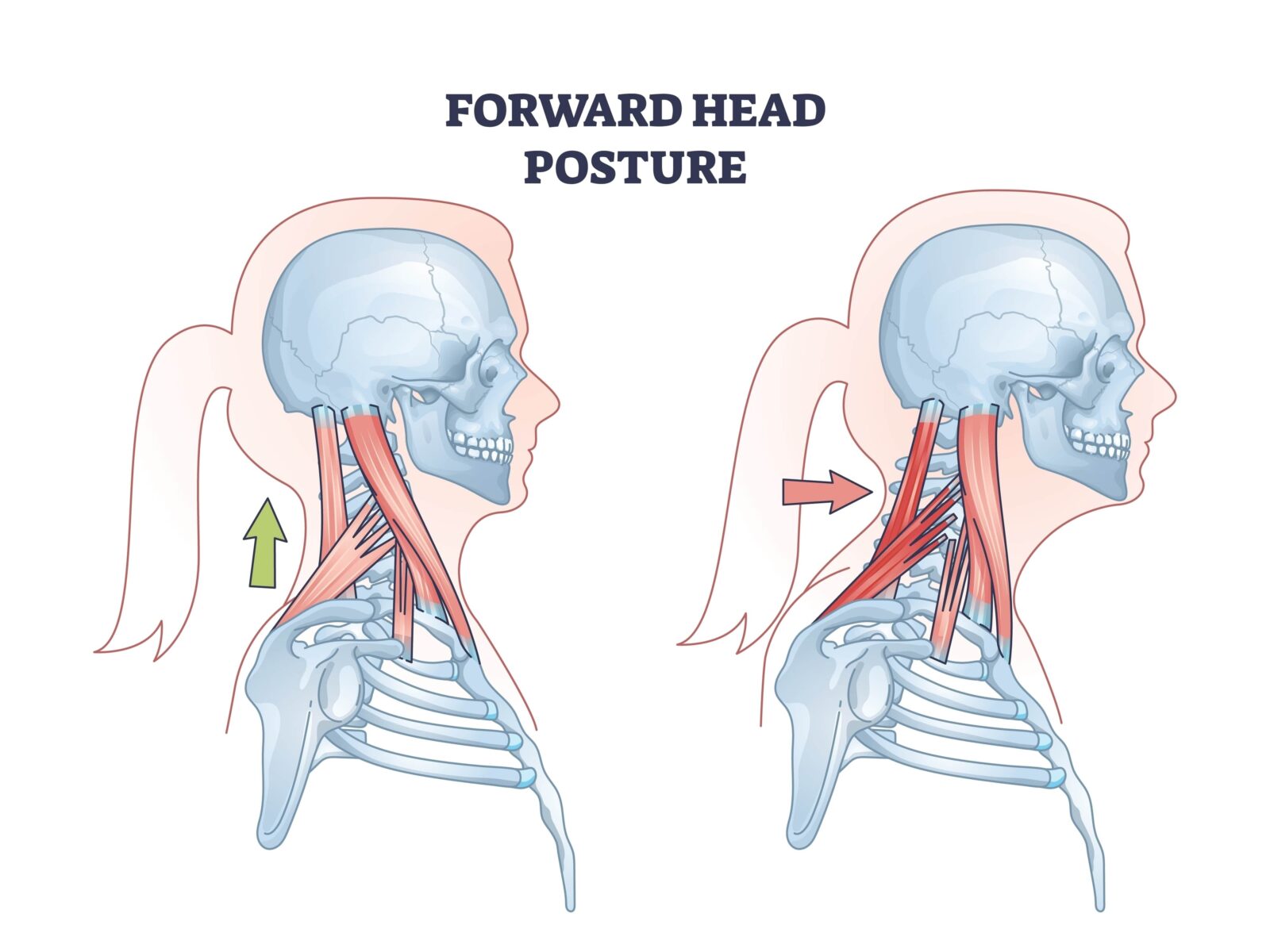
- Muscle Tension and Posture: Muscle tension and poor posture are common contributors to both neck pain and headaches. For instance, prolonged periods of poor posture, such as hunching over a computer or phone, can strain the neck muscles, leading to neck pain, which may then trigger headaches. Similarly, stress and anxiety can cause muscle tension in the neck, contributing to both neck pain and headaches.
- Joint Dysfunction and Injuries: Injuries to the neck, such as whiplash from a car accident or sports-related trauma, can lead to both neck pain and headaches. Additionally, dysfunction in the small facet joints of the cervical spine can cause pain in the neck that radiates to the head.
- Vascular and Circulatory Issues: Some headaches, like migraines, have complex origins involving changes in blood flow to the brain. Neck pain can sometimes be associated with vascular issues, which might also contribute to certain types of headaches.
- Underlying Conditions: Certain underlying conditions, such as herniated discs, degenerative disc disease, or spinal stenosis in the neck, can cause both neck pain and headaches. The structural issues can put pressure on nerves and lead to referred pain in the head.
Available Treatments from a Spinal Specialist
Consulting a spinal specialist or a spine-focused healthcare professional is crucial to accurately diagnose and treat headaches arising from neck pain. The specialist will conduct a comprehensive evaluation, including a medical history review and physical examination, to identify the root cause of the headaches. Based on the diagnosis, the specialist may recommend the following treatments:
Medications:
Spinal specialists may prescribe medications to manage pain, reduce inflammation, and improve overall spinal health. The types of medications prescribed may include:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These drugs help reduce inflammation and provide pain relief.
- Muscle Relaxants: Used to alleviate muscle spasms and tension in the spine.
- Pain Relievers: Over-the-counter or prescription pain medications may be prescribed for short-term pain relief.
- Corticosteroids: In certain cases of severe inflammation, oral or injectable corticosteroids may be administered to reduce swelling and pain.
Physical Therapy:
Physical therapy is a cornerstone of spinal treatment. A spinal specialist may refer patients to a physical therapist who specializes in spine-related conditions. Physical therapy aims to strengthen the muscles supporting the spine, improve flexibility, correct posture, and teach patients exercises to manage pain and prevent further issues.
Spinal Injections:
For more severe or persistent pain, spinal injections may be recommended. These injections deliver medications directly to the affected area of the spine to reduce inflammation and alleviate pain. Common types of spinal injections include:
- Epidural Steroid Injections (ESIs): Delivered into the epidural space of the spine to reduce inflammation and pain associated with nerve compression.
- Facet Joint Injections: Targeting the small joints in the spine to relieve pain and diagnose the source of the pain.
- Nerve Root Blocks: Used to treat pain caused by irritation or compression of specific spinal nerves.
Spinal Cord Stimulation:
Spinal cord stimulation (SCS) is a pain management technique that involves the implantation of a small device under the skin. The device sends electrical impulses to the spinal cord, which can interfere with pain signals, reducing the sensation of pain. SCS is often considered for chronic pain conditions that have not responded to other treatments.
Spinal Surgery:
When conservative treatments fail to provide relief or when the spinal condition is severe and requires intervention, a spinal specialist may recommend surgery. Spinal surgery aims to address structural issues in the spine, decompress nerves, stabilize the spine, and correct deformities. Some common types of spinal surgeries include:
- Discectomy: Removal of a herniated or damaged disc that is pressing on a nerve.
- Laminectomy: The removal of the lamina (part of the vertebral arch) to relieve pressure on the spinal cord or nerves.
- Spinal Fusion: Joining two or more vertebrae together to stabilize the spine and reduce pain.
- Artificial Disc Replacement: Replacing a damaged disc with an artificial one to maintain spinal flexibility.
It’s important to note that each patient’s condition is unique, and the treatment plan will be tailored to their specific needs and medical history. Spinal specialists work closely with patients to determine the most appropriate and effective course of action to alleviate pain, improve function, and enhance overall quality of life.
Preventing Headaches from Neck Pain
Prevention is always better than cure. To reduce the risk of headaches arising from neck pain, consider the following preventive measures:
- Maintain Good Posture: Be mindful of your posture during daily activities, especially while working at a desk or using electronic devices.
- Stay Active: Regular exercise can help keep the neck muscles strong and flexible.
- Stress Management: Adopt stress-reducing techniques such as meditation, yoga, or deep breathing exercises.
- Ergonomic Workspace: Ensure your workspace is ergonomically designed to minimize strain on the neck and spine.
In Conclusion
Headaches originating from neck pain can significantly impact one’s quality of life if left untreated. Consulting a spinal specialist is essential to accurately diagnose the underlying cause and develop a personalized treatment plan. By understanding the link between neck pain and headaches and exploring available treatments, individuals can find relief and improve their overall well-being. Remember to prioritize prevention through lifestyle adjustments and proper self-care to minimize the risk of future headaches stemming from neck pain.