Maintaining optimal spinal health is crucial for overall well-being, as the spine plays a vital role in supporting our body and facilitating movement. Among the various conditions that can affect the spine, herniated and bulging discs are two commonly encountered issues. In this article, we will explore the key differences between these conditions, shedding light on their causes, symptoms, diagnosis, and treatment options.
Spinal Anatomy and Disc Structure
The spine, also known as the vertebral column, is a complex structure consisting of a series of bones called vertebrae. The spinal column serves as the central support for the body and protects the delicate spinal cord. Between each pair of vertebrae lies an intervertebral disc, which plays a crucial role in spinal anatomy. These discs act as shock absorbers, cushioning the vertebrae during movement and preventing bone-on-bone contact. Each intervertebral disc has a unique structure, comprising two main components: the outer annulus fibrosus and the inner nucleus pulposus. The annulus fibrosus is a tough, fibrous outer layer that encases the nucleus pulposus, a gel-like substance at the center of the disc. This structure provides stability, flexibility, and elasticity to the spine, allowing for various movements while maintaining its overall integrity. The spinal anatomy and disc structure work in harmony to support the body’s weight, facilitate movement, and protect the spinal cord and nerves.
Bulging Disc
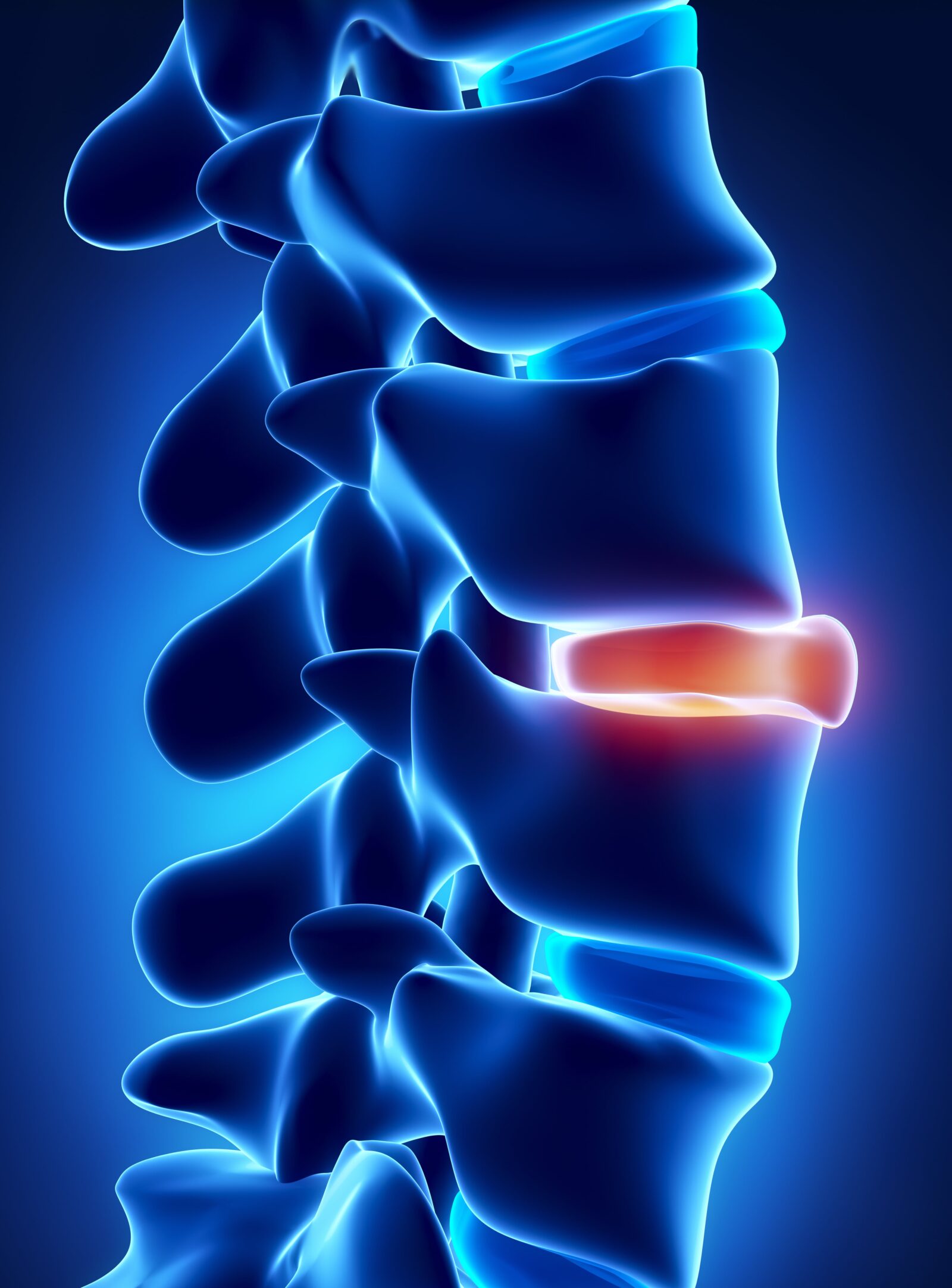
A bulging disc occurs when the disc protrudes outwards beyond its normal position, typically due to age-related degeneration or wear and tear. It is important to note that a bulging disc is not considered a herniation. Instead, it signifies a disc that has shifted or bulged, potentially causing discomfort or pain.
Symptoms of a bulging disc may include localized pain, numbness, or tingling sensations in the affected area. However, the severity of symptoms can vary from person to person. Diagnosis typically involves a physical examination, imaging tests such as MRI or CT scans, and a comprehensive evaluation by a medical professional.
Treatment for a bulging disc often involves non-surgical approaches. These may include rest, physical therapy, exercises to strengthen the surrounding muscles, and pain management techniques. In severe cases where conservative methods fail to alleviate symptoms, surgical interventions such as discectomy or microdiscectomy may be considered.
Herniated Disc
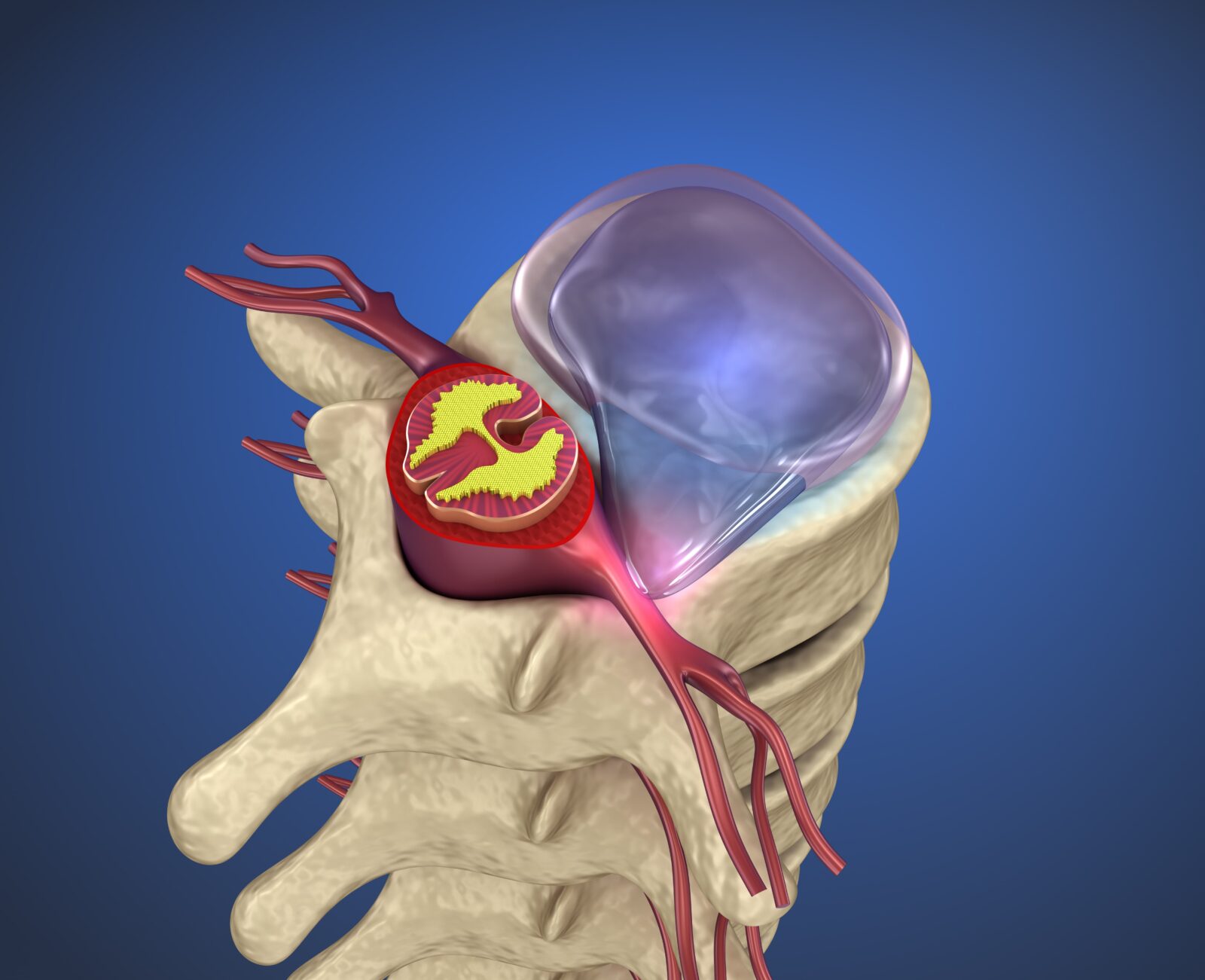
A herniated disc, also known as a slipped or ruptured disc, occurs when the inner gel-like nucleus pulposus breaks through the outer annulus fibrosus. This can be caused by trauma, lifting injuries, or degenerative conditions. Unlike a bulging disc, a herniated disc involves the actual rupture or tearing of the disc’s structure.
The symptoms of a herniated disc may vary depending on the location and extent of the herniation. Common signs include localized or radiating pain, muscle weakness, and numbness or tingling in the affected area. Diagnosis involves a thorough physical examination, imaging tests, and neurological assessments to evaluate nerve function.
Treatment for a herniated disc typically begins with conservative methods such as rest, physical therapy, pain medications, and epidural injections to reduce inflammation and manage symptoms. In cases where conservative treatments fail or when there is severe pain or nerve compression, surgical options such as discectomy, laminectomy, or spinal fusion may be recommended.
Key Differences Between Herniated and Bulging Discs
Understanding the distinctions between herniated and bulging discs is essential. Overall, the key differences between a herniated and bulging disc lie in the severity of the structural damage, the intensity of symptoms, and the treatment approaches. A herniated disc involves a complete rupture or tear of the disc and may cause more pronounced symptoms, requiring a range of treatment options. On the other hand, a bulging disc involves a shift or bulge of the disc without a complete rupture and often results in milder symptoms that can be managed with conservative methods.
Here’s the information organized into a table for a clear visual comparison:
| Herniated Disc | Bulging Disc | |
| Definition | Inner gel-like nucleus pulposus breaks through annulus fibrosus, resulting in a rupture or tear of the disc’s structure. | Disc shifts or bulges outwards beyond its normal position without a complete rupture or tear of the disc’s structure. |
| Severity | More significant and complete disruption of the disc’s structure. | Less severe condition as the outer layer of the disc remains intact. |
| Symptoms | Localized or radiating pain, muscle weakness, numbness, or tingling sensations. | Localized pain, discomfort, or numbness (may be milder or absent in some cases). |
| Diagnostic Imaging | MRI or CT scans can identify the location and severity of the herniation. | MRI or CT scans visualize the bulging disc and assess its size and impact. |
| Treatment Options | Conservative methods (rest, physical therapy, pain medications, epidural injections) or surgical intervention (discectomy, laminectomy, spinal fusion) in severe cases. | Non-surgical approaches (rest, physical therapy, exercises, pain management) with rare surgical intervention in severe cases. |
By comparing the information side by side in a table format, it becomes easier to understand and distinguish the key differences between a herniated disc and a bulging disc.
Spinal Surgery for Herniated or Bulging Discs
Spinal surgery can be an option for treating herniated or bulging discs in certain cases where conservative treatments have been unsuccessful or when there is severe pain, neurological deficits, or compression of nerves or the spinal cord. The specific type of surgery will depend on the individual’s condition and the severity of the disc issue.
For herniated discs, a common surgical procedure is a discectomy. During a discectomy, the surgeon removes a portion or the entire herniated disc to relieve pressure on the nerves or spinal cord. In some cases, a microdiscectomy may be performed, which involves a minimally invasive technique using smaller incisions and specialized instruments.
In more complex cases or when there are multiple affected discs, other surgical options such as laminectomy, laminotomy, or spinal fusion may be considered. A laminectomy involves removing part of the lamina (the bony arch) to create more space for the compressed nerves. Laminotomy is a similar procedure but involves removing a smaller portion of the lamina. Spinal fusion involves joining two vertebrae together, usually using bone grafts or metal implants, to stabilize the spine.
For bulging discs, surgical intervention is less common compared to herniated discs. However, in cases where conservative treatments have not provided relief or if the bulging disc is causing severe pain or nerve compression, surgical options such as discectomy or spinal fusion may be considered to address the underlying issue.
It’s important to note that surgery is typically considered after non-surgical treatments have been explored, and the decision to undergo spinal surgery should be made in consultation with a qualified healthcare professional who can evaluate the individual’s specific condition and recommend the most appropriate course of treatment.
In Conclusion
Herniated and bulging discs are common spinal conditions that can cause discomfort and impact daily life. By understanding the key differences between these conditions, individuals can seek appropriate medical advice and receive tailored treatment plans. It is crucial to consult with a healthcare professional for an accurate diagnosis and guidance regarding the best course of action. Early intervention and proactive measures for spinal health can contribute to long-term well-being and an active lifestyle.

