Osteoporosis, a silent yet pervasive condition, significantly impacts spine health, leading to debilitating consequences if left unchecked. Characterized by porous and fragile bones, osteoporosis makes individuals prone to fractures, particularly in the spine, which can result in severe pain and reduced mobility. With the spine acting as the body’s central support structure, its vulnerability to osteoporotic damage underscores the need for vigilant prevention and management strategies. This blog delves into the intricacies of osteoporosis and its implications for spinal health, highlighting the importance of early detection, preventative measures, and the latest treatment options. Through a comprehensive exploration of causes, symptoms, and innovative treatments, we aim to equip readers with the knowledge and tools necessary to safeguard their spine health against the stealthy advance of osteoporosis.
Understanding Osteoporosis
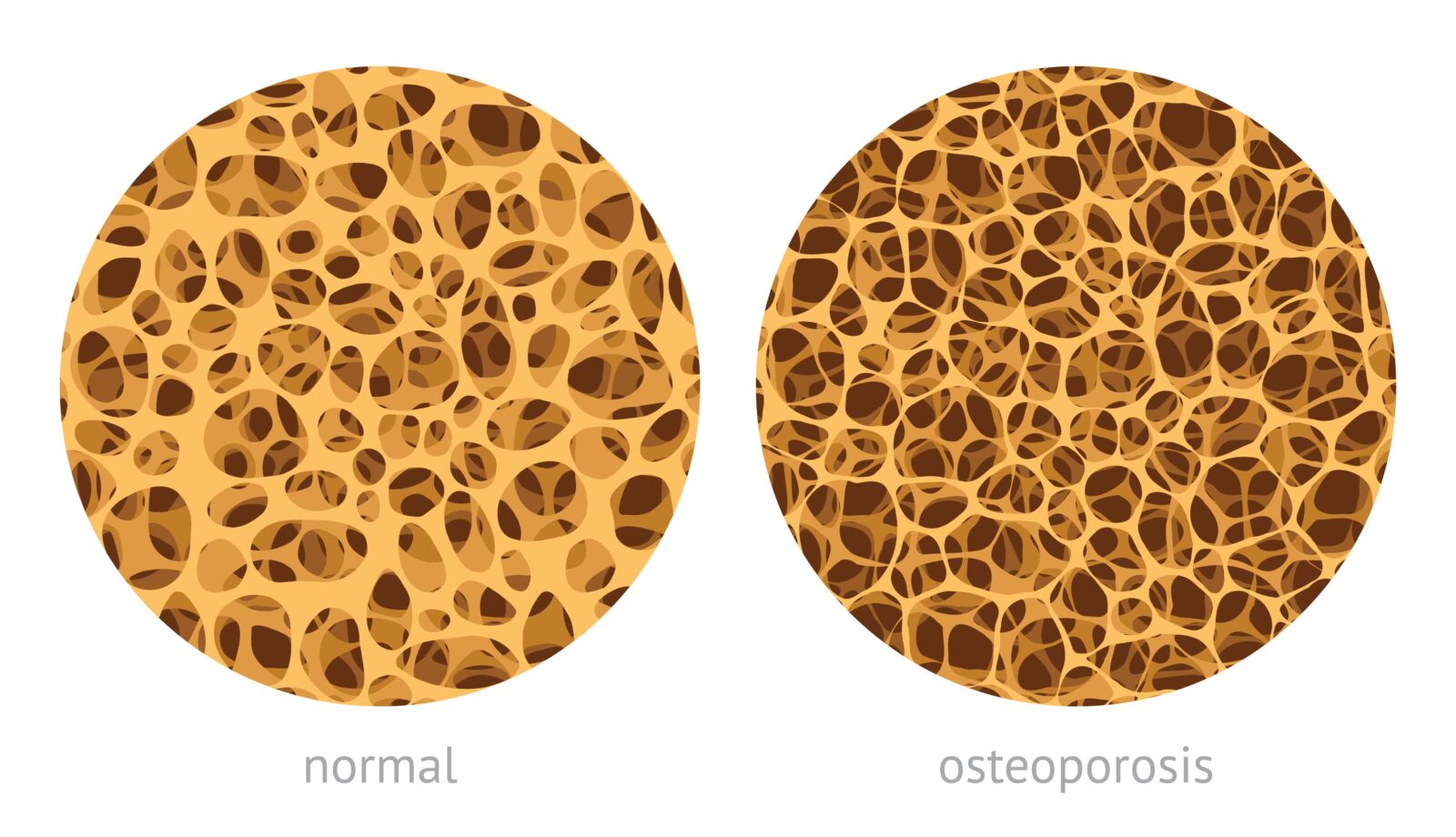
Osteoporosis is a bone disease characterized by a decrease in bone density and strength, leading to bones that are fragile and more prone to fractures. It often progresses without any symptoms until a bone fracture occurs, typically in the wrist, hip, or spine. The disease primarily affects older adults, particularly postmenopausal women, but can also affect men and younger individuals under certain conditions.
Causes and Risk Factors
The exact cause of osteoporosis is multifactorial, involving genetic, hormonal, dietary, and lifestyle influences. Key risk factors include:
- Age: The risk increases as you get older, due to the natural decline in bone density.
- Gender: Women are more susceptible, especially after menopause due to the decrease in estrogen, a hormone important for bone health.
- Family history: A family history of osteoporosis or bone fractures can increase risk.
- Nutritional deficiencies: Lack of calcium and vitamin D can lead to weaker bones.
- Lifestyle choices: Smoking, excessive alcohol consumption, and a sedentary lifestyle contribute to bone loss.
Signs and Symptoms
In the early stages, osteoporosis may not cause any symptoms. However, as the condition progresses, it can lead to noticeable changes, especially in spine health.
- Back pain: Originating from fractured or weakened vertebrae.
- Reduction in height: Cumulative loss of height over time due to compression fractures in the spine.
- Postural changes: Stooped posture or kyphosis may develop as a result of spinal bone loss.
- Frequent fractures: The spine becomes so fragile that fractures can occur with minor stresses, such as bending, lifting, or even coughing.
- Severe back pain: Chronic pain that worsens with movement and may improve when lying down.
- Limited mobility: Difficulty in performing daily activities due to pain and spinal deformity.
Diagnosis and Screening
Early detection of osteoporosis is crucial for effective management and treatment, which can significantly reduce the risk of fractures, especially in the spine. Regular medical check-ups can help detect osteoporosis before a fracture occurs. Discussing personal risk factors with a healthcare provider can lead to early screening and intervention.
Diagnostic Tests
- Bone Density Test (DEXA scan): The most common test used to diagnose osteoporosis, measuring bone mineral density (BMD).
- Spinal X-rays: Can detect vertebral fractures and help assess the severity of osteoporosis.
- CT scans and MRI: Used in certain cases to provide more detailed images of the bones and tissues.
Interpreting Test Results
The results of a bone density test are usually given as a T-score, which compares the bone density with that of a healthy young adult. A T-score of -1.0 or above is considered normal, between -1.0 and -2.5 indicates low bone mass (osteopenia), and -2.5 or below signifies osteoporosis. Early diagnosis and appropriate treatment can help manage the condition effectively and prevent serious complications related to spine health.
Prevention Strategies
Preventing osteoporosis, especially to protect spine health, involves a combination of lifestyle choices, dietary adjustments, and regular health screenings. By taking proactive measures, individuals can significantly reduce their risk of developing osteoporosis and experiencing related spinal fractures.
Dietary Recommendations

- Calcium and Vitamin D: These are crucial for bone health. Dairy products, green leafy vegetables, fish, and fortified foods are excellent sources of calcium, while vitamin D can be obtained from sunlight exposure, fatty fish, and fortified foods.
- Protein: Adequate protein intake is essential for bone strength. Sources include lean meats, beans, nuts, and dairy products.
- Limiting caffeine and alcohol: Excessive consumption can interfere with bone density.
Exercise and Physical Activity
- Weight-bearing exercises: Activities like walking, jogging, and dancing help build and maintain bone density.
- Strength training: Lifting weights or using resistance bands can strengthen the muscles and bones in the spine and throughout the body.
- Balance and flexibility exercises: Yoga and tai chi can improve balance, reduce the risk of falls, and support spine health.
Lifestyle Modifications
- Smoking cessation: Smoking is known to accelerate bone loss.
- Moderation in alcohol consumption: Excessive alcohol can lead to bone loss and increase the risk of falls.
- Fall prevention measures: Ensuring a safe living environment to reduce the risk of falls that can cause fractures.
Treatment Options
Once osteoporosis is diagnosed, treatment focuses on slowing bone loss, preventing fractures, and managing symptoms, particularly to protect the spine.
Medications
- Bisphosphonates: Commonly prescribed for osteoporosis, these drugs help prevent bone loss and reduce the risk of fractures.
- Hormone-related therapy: For postmenopausal women, medications that mimic estrogen can help maintain bone density.
- Calcium and vitamin D supplements: Often recommended to ensure adequate intake for bone health.
Non-pharmacological Treatments
- Physical therapy: Tailored exercises can strengthen the muscles supporting the spine, improve balance, and reduce the risk of falls.
- Orthopedic supports: Braces or supports can help stabilize the spine and relieve pain.
Surgical Options
For severe cases, especially where fractures lead to significant spinal deformity or chronic pain, surgical interventions may be considered:
- Vertebroplasty and kyphoplasty: Procedures that involve injecting cement-like material into the fractured vertebrae to stabilize the spine and relieve pain.
- Spinal fusion surgery: Involves joining two or more vertebrae together to limit movement and provide stability to the spine.
Treatment plans are tailored to individual needs, based on the severity of osteoporosis, the risk of fractures, and overall health. Regular monitoring and adjustments to the treatment regimen are essential to effectively manage osteoporosis and protect spine health.
Conclusion
In conclusion, understanding and addressing osteoporosis is crucial for maintaining spine health and overall quality of life. Early detection, preventive strategies, and effective treatment plans are key to managing this silent yet impactful condition. By incorporating healthy dietary choices, engaging in regular exercise, making lifestyle adjustments, and following medical guidance, individuals can significantly reduce their risk of osteoporotic fractures and maintain a strong, healthy spine. As research advances, new treatments continue to emerge, offering hope for improved outcomes. It is essential for individuals, especially those at higher risk, to stay informed and proactive in their approach to bone health, ensuring a robust and resilient framework for life.










