The spine is an intricate structure composed of bones, muscles, and ligaments, pivotal in providing support and flexibility to the human body. Central to this function are the spinal discs, which act as shock absorbers between the vertebrae, allowing for smooth movements and helping bear the body’s weight. However, these discs can succumb to various issues, such as herniation, degeneration, and bulging, leading to discomfort and debilitating pain. Understanding these common spinal disc problems is crucial for effective prevention and management. In this blog, we’ll delve into the anatomy of spinal discs, explore the symptoms and diagnostic methods for different disc issues, and discuss a range of treatment options from physical therapy to surgery, aiming to provide valuable insights for those suffering from this challenging condition.
Understanding Spinal Disc Problems
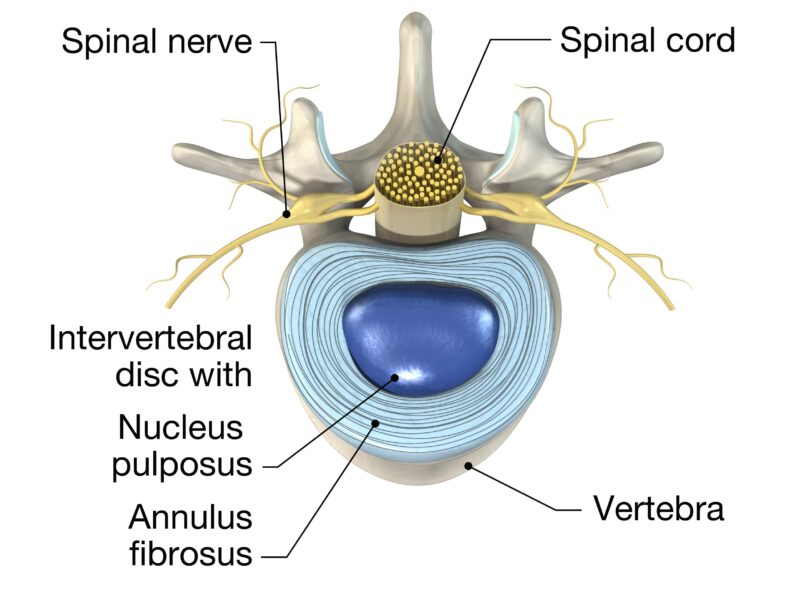
A spinal disc is a small, doughnut-shaped structure located between the vertebrae, the series of bones that make up the spinal column. Each disc consists of two main parts: the nucleus pulposus and the annulus fibrosus. The nucleus pulposus at the center is soft and gelatinous, designed to absorb shocks and pressures exerted on the spine during activities like walking, running, or lifting. Surrounding the nucleus is the annulus fibrosus, a tough, rubbery ring that provides structure and strength to the disc, keeping the nucleus contained and functioning effectively. Common spinal disc problems include:
Herniated Disc:
This condition occurs when the nucleus pulposus breaks through the annulus fibrosus due to wear, tear, or injury. This rupture can put pressure on the nearby nerve roots or spinal cord, leading to pain, numbness, or weakness in the limbs or torso. Herniated discs are more commonly found in the lumbar region but can occur anywhere along the spine.
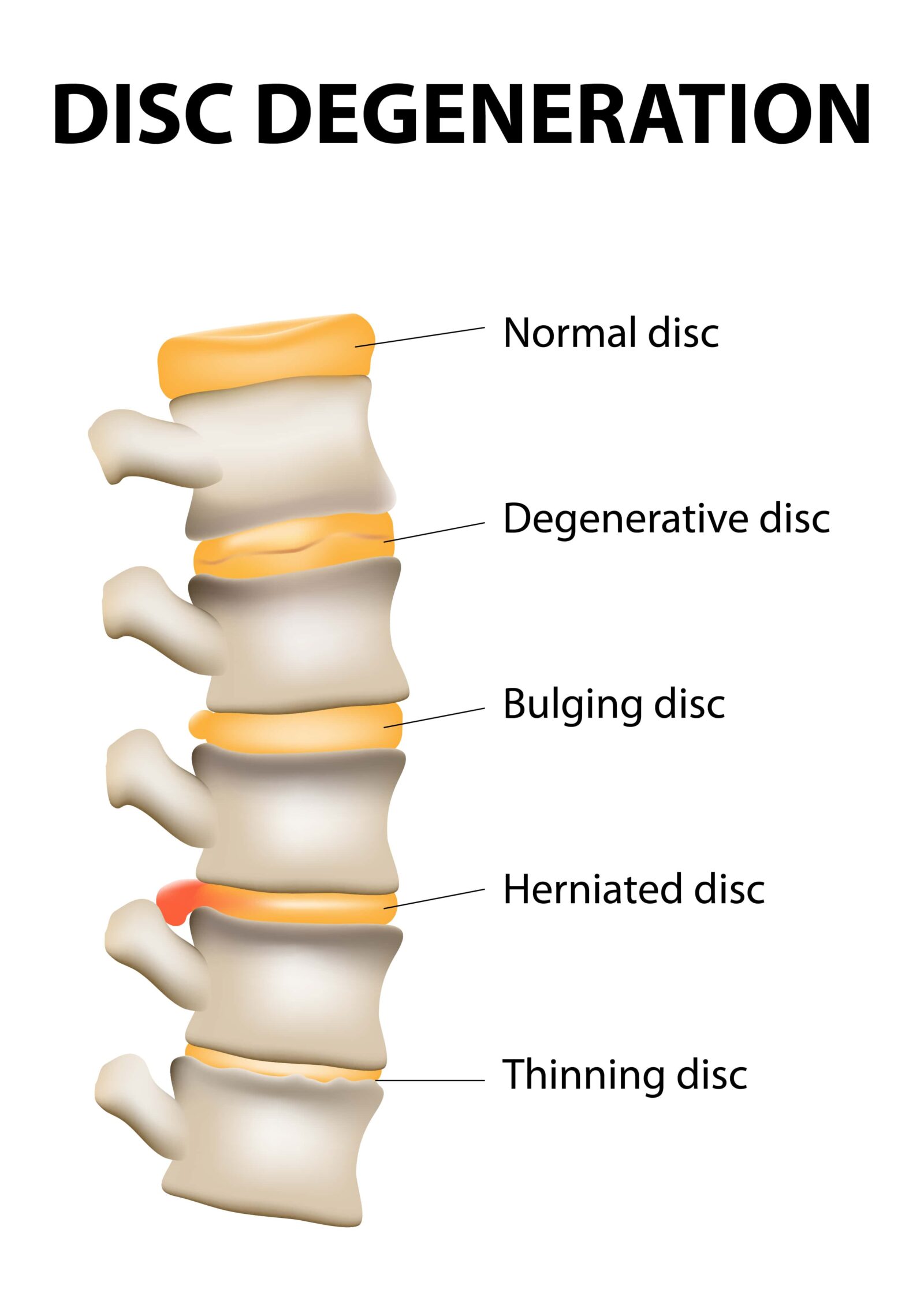
Degenerative Disc Disease:
As we age, our spinal discs naturally lose fluid and become less flexible, reducing their ability to cushion the vertebrae and more susceptible to tearing. This process can lead to chronic back pain, instability, and reduced mobility. Degenerative changes are a normal part of aging, but for some, it leads to significant discomfort and impairment.
Bulging Disc:
Unlike a herniated disc, where the disc material breaks through the annulus fibrosus, a bulging disc refers to the disc stretching and protruding outward without breaking the outer ring. This bulge can still compress spinal nerves, causing pain and discomfort, typically occurring as a result of age-related wear or stress on the spine.
Understanding these issues is the first step in recognizing the signs and seeking appropriate treatment before complications arise. Early intervention can significantly improve outcomes, making knowledge of these conditions vital for maintaining spinal health.
Symptoms of Spinal Disc Issues
Spinal disc problems can manifest in a variety of symptoms, which may differ depending on the location and severity of the issue. Recognizing these symptoms is crucial for timely diagnosis and treatment.
General Symptoms:
The most common signs of disc problems include pain that can be localized or radiating, numbness, and a tingling sensation. Some people may also experience muscle weakness or stiffness in the affected area. The pain might worsen with movements such as bending over, lifting heavy objects, or sitting for prolonged periods.
Symptoms by Location:
- Cervical (Neck): Issues in the cervical discs can cause pain and stiffness around the neck, which might extend to the arms, shoulders, or even result in headaches.
- Thoracic (Mid-back): Thoracic disc problems are less common but can cause pain in the middle of the back. In some cases, the pain may radiate around the chest, which can sometimes be mistaken for heart-related issues.
- Lumbar (Lower back): This is the most common area for disc problems due to the high degree of stress and movement. Symptoms include lower back pain, sciatica (a sharp, shooting pain through the buttocks and down one leg), and even changes in reflexes.
When to Seek Medical Advice:
It is important to consult a healthcare provider if the pain:
- Is persistent and does not improve with rest.
- Is severe and inhibits daily activities.
- Is accompanied by symptoms such as significant leg weakness, loss of bladder or bowel control, or severe, sudden pain in both legs.
These symptoms can indicate a more serious condition requiring immediate medical attention, such as cauda equina syndrome. Early detection and treatment are vital to prevent further damage and improve the quality of life.
Diagnosing Spinal Disc Problems
Accurately diagnosing spinal disc issues is essential for effective treatment and management. Here’s how medical professionals typically diagnose these conditions:
Diagnostic Tools
- MRI (Magnetic Resonance Imaging): This is the most commonly used diagnostic tool for spinal disc problems. MRI scans provide detailed images of the body’s soft tissues, including the spinal discs and nerves. They can show the exact location and severity of the disc damage.
- CT Scan (Computed Tomography): A CT scan can provide a good image of the bone architecture of the spine and is often used when more detail about the vertebrae is needed.
- X-rays: While not as detailed for soft tissue injuries like disc problems, X-rays can help rule out other causes of back pain, such as fractures or tumors.
Physical Examination
During the physical exam, a doctor will check for areas of tenderness, the range of motion, and the nerve function in your arms and legs. Reflex tests, muscle strength comparisons, and pain response tests are typical during this examination.
Patient History
A thorough patient history is crucial for diagnosing spinal disc problems. Doctors will ask about the onset, duration, and severity of symptoms, as well as any previous injuries or activities that may have led to the condition. Understanding family medical history can also provide insights into hereditary aspects of spinal issues.
Importance of Early Diagnosis
Early diagnosis can prevent the progression of disc damage and alleviate symptoms before they become more severe. Delayed treatment can lead to chronic pain, irreversible nerve damage, or even permanent disability. Additionally, identifying the specific type of disc problem can help tailor the treatment plan to be more effective, whether it involves conservative measures like physical therapy or more invasive procedures like surgery.
This comprehensive approach to diagnosis helps ensure that all potential causes of symptoms are considered and that the treatment plan addresses the specific needs of the patient, leading to better outcomes.
Treatment Options
Effective treatment for spinal disc problems can vary widely depending on the severity and location of the issue, as well as the individual’s overall health and lifestyle. Here’s a breakdown of the various treatment options available:
Non-Surgical Treatments
Non-surgical options are typically the first line of treatment for spinal disc issues, especially when symptoms are mild to moderate.
- Physical Therapy: Physical therapists can design personalized exercise programs that help strengthen the muscles around the spine, improve flexibility, and reduce pressure on the spinal discs. Techniques such as traction, massage, and ultrasound may also be used to alleviate pain.
- Medications: Pain relief medications, such as NSAIDs (non-steroidal anti-inflammatory drugs), can help reduce inflammation and pain. In some cases, muscle relaxants or nerve pain medications, like gabapentin, are prescribed to manage symptoms.
- Injections: Corticosteroid injections can be administered directly into the area around the spinal nerves, which can significantly reduce inflammation and pain. This treatment is usually considered when pain does not respond well to other non-surgical treatments.
Surgical Treatments
Surgery may be considered when non-surgical treatments fail to relieve symptoms, or if the nerve compression leads to significant weakness, loss of function, or other serious symptoms.
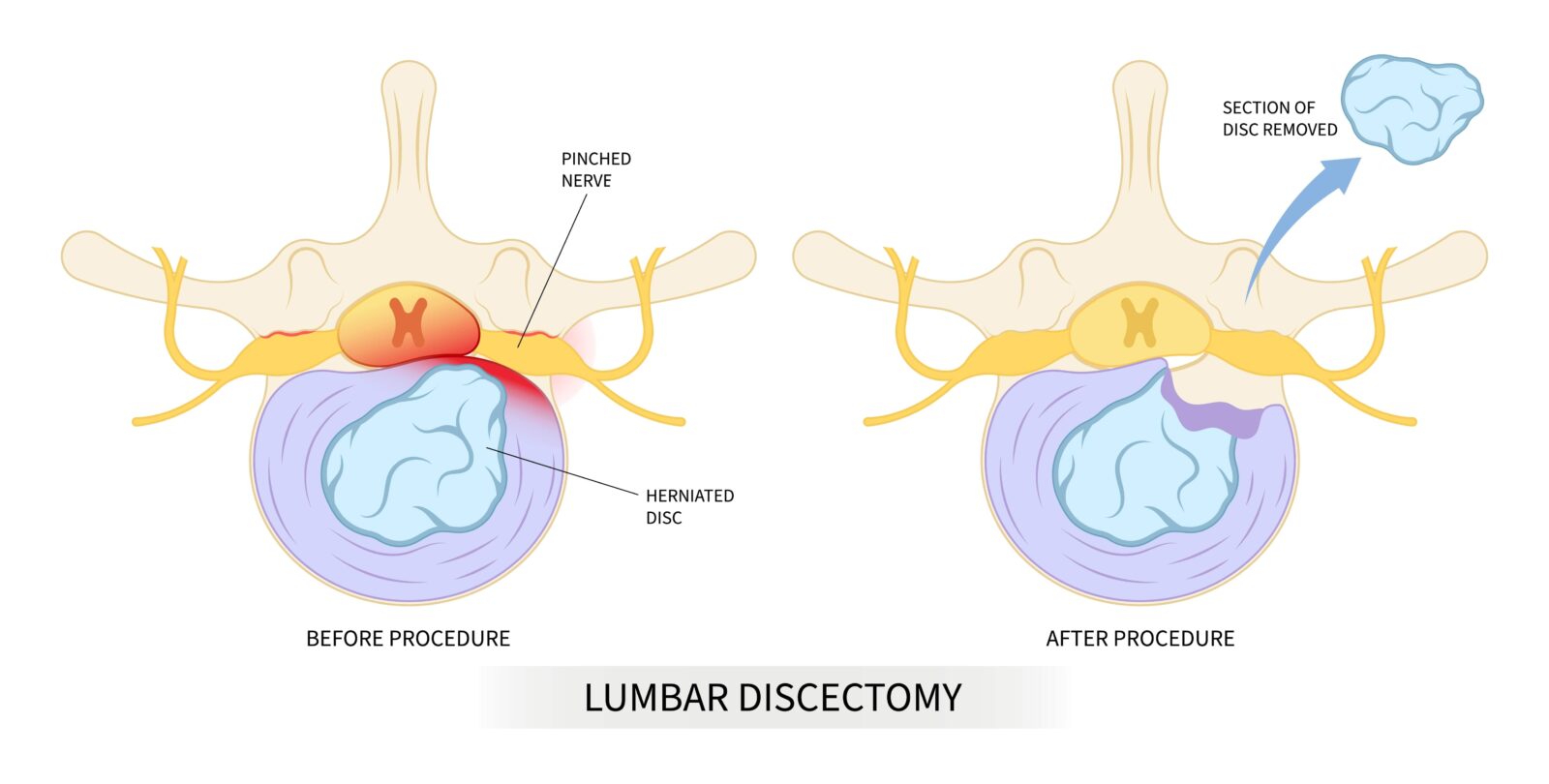
- Discectomy: This involves the removal of a portion of the herniated disc to relieve pressure on the nearby nerves.
- Laminectomy: The removal of part of the bone, the lamina, from the affected vertebra to create more space for the nerves.
- Spinal Fusion: Fusing two or more vertebrae together to stabilize the spine. This is often done after removing a damaged disc.
Alternative Treatments
Some patients may find relief through alternative therapies, although these should be pursued in consultation with a healthcare professional.
- Acupuncture: This traditional Chinese medicine technique involves inserting fine needles into specific points on the body, which may help relieve pain and improve function.
- Chiropractic Care: Chiropractors can perform adjustments to help improve spinal function and alleviate stress on your system.
- Yoga: Certain yoga poses can improve flexibility, strengthen the back muscles, and reduce stress, which might help relieve some back pain symptoms.
Lifestyle Changes
In addition to medical treatments, making lifestyle changes can play a crucial role in managing and preventing disc problems.
- Ergonomic Adjustments: Improving posture and ergonomics at work or during other activities can help reduce the risk of disc injuries.
- Exercise: Regular, low-impact exercise helps keep the back muscles strong and flexible, which can prevent further injuries and help support the spine.
Conclusion
In conclusion, understanding spinal disc problems and their diverse treatment options is essential for managing and alleviating the symptoms associated with these conditions. By familiarizing oneself with the anatomy, symptoms, and diagnostic approaches, individuals can take proactive steps towards early detection and effective management. Whether through non-surgical methods, surgical interventions, or lifestyle changes, each treatment strategy offers a pathway to relief and recovery. It is crucial for those experiencing back pain or related symptoms to seek professional advice, ensuring personalized care tailored to their specific needs. Ultimately, maintaining a healthy spine is integral to overall well-being, underscoring the importance of prevention, timely intervention, and sustained management of spinal health.