Scoliosis, a complex spinal deformity characterized by a sideways curvature of the spine, is not just a condition affecting children; it is also prevalent among adults. While adolescent scoliosis often garners more attention, adult scoliosis can significantly impact one’s quality of life through pain, reduced mobility, and other health challenges. This blog aims to explore the various facets of adult scoliosis, including its types, symptoms, diagnosis, and the range of treatment options available. Understanding these aspects is vital for managing the condition effectively and improving overall well-being. Here, we will also highlight supportive resources and coping strategies to assist adults living with scoliosis in leading more comfortable and fulfilling lives.
Understanding Scoliosis in Adults
Scoliosis in adults is a condition that remains relatively misunderstood by many. It involves a curvature of the spine that is either a continuation of an issue identified in childhood or one that develops due to age-related spinal degeneration. Understanding the nature and types of adult scoliosis is crucial for effective management and treatment. Adult scoliosis is primarily categorized into two types:
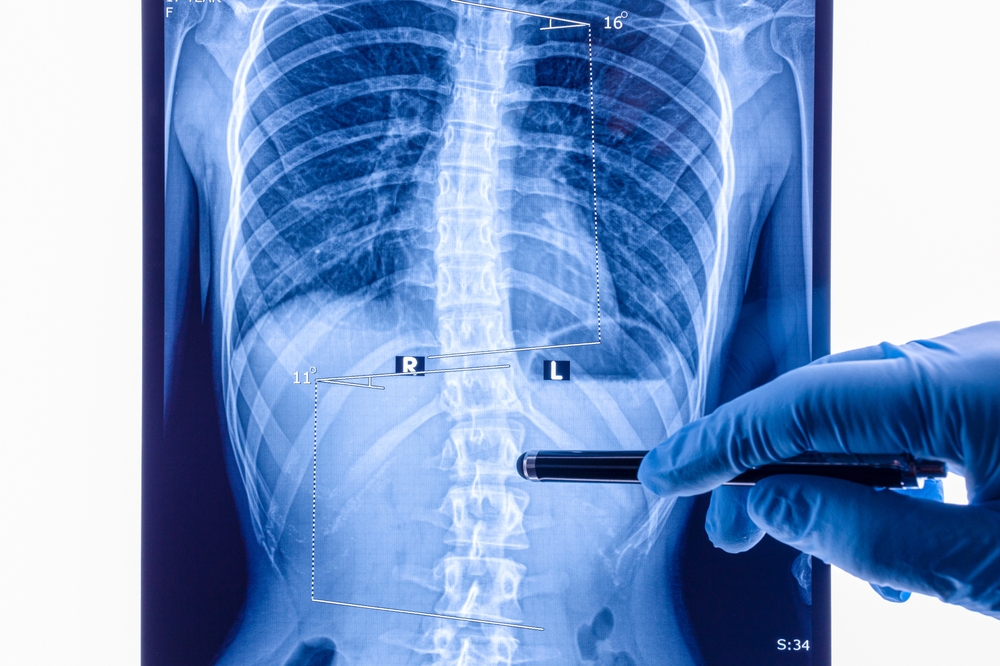
Adult Idiopathic Scoliosis:
This type originates in childhood but may not become symptomatic or require treatment until adulthood. It is a continuation of adolescent idiopathic scoliosis where the initial curvature worsens or begins causing problems as the individual ages.
De Novo or Adult Degenerative Scoliosis:
Unlike idiopathic scoliosis, de novo scoliosis begins in adulthood. It is typically caused by the degeneration of the spinal discs and joints, leading to an asymmetric alignment of the spine. This type is most common in people over the age of 50 and can be exacerbated by osteoporosis, vertebral fractures, or arthritis.
Symptoms of Adult Scoliosis
The symptoms of adult scoliosis can vary significantly depending on the severity and location of the spine curvature. Common symptoms include:
- Chronic back pain: This is often the primary complaint due to the abnormal spinal alignment and the stress it places on muscles, nerves, and ligaments.
- Stiffness and reduced mobility: As the spine becomes more curved, it can lead to a decrease in flexibility, affecting daily activities.
- Numbness, tingling, or weakness: These symptoms can occur if the spinal curvature leads to nerve compression.
- Visible changes in posture: This may include a noticeable lean to one side, uneven shoulders or hips, or a prominent rib hump.
Understanding these symptoms is essential not just for diagnosis but also for deciding on the course of treatment, as the presence and severity of symptoms often guide therapeutic decisions.
Diagnosing Adult Scoliosis
Diagnosis of adult scoliosis typically involves a combination of physical examination and imaging studies. During a physical exam, a healthcare provider will look for visible signs of scoliosis such as asymmetry in the shoulders, waist, or hips. They may also observe the spine’s alignment while the patient stands and bends forward.
Imaging tests play a crucial role in diagnosing scoliosis in adults:
- X-rays: These are the most common form of imaging used to confirm a diagnosis of scoliosis, allowing doctors to see the spine’s curvature and measure its angle.
- MRI or CT scans: These can be used to assess more complex cases and evaluate the spine for any nerve compression or other abnormalities that may be causing symptoms.
Early detection is vital in managing adult scoliosis effectively, as it allows for timely intervention before symptoms worsen or lead to significant complications. Understanding the nature of scoliosis, its symptoms, and diagnostic methods sets the foundation for exploring the treatment options.
Treatment Options for Adult Scoliosis
Adult scoliosis can vary greatly in terms of severity and the impact on daily life, which means treatment plans need to be personalized. Treatment options range from conservative approaches aimed at managing symptoms to more invasive surgical interventions to correct spinal deformities. Below, we explore these varied treatment strategies for adult scoliosis.
Non-Surgical Treatments
For many adults with scoliosis, non-surgical treatment methods are the first line of defense. These options focus on relieving symptoms, improving functional abilities, and slowing the progression of the spinal curve.
- Physical Therapy: Physical therapists can develop tailored exercise programs that strengthen core muscles, improve spinal alignment, and enhance flexibility. These exercises are designed not only to reduce pain but also to improve posture and decrease the risk of the curvature worsening.
- Pain Management: Chronic pain associated with scoliosis can often be managed through various non-invasive methods:
- Medications: Over-the-counter pain relievers like ibuprofen or acetaminophen may be recommended. In more severe cases, prescription medications may be used.
- Injections: Corticosteroid injections can provide temporary relief from inflammation and pain in the spine.
- Alternative Therapies: Acupuncture, chiropractic treatments, and massage therapy have also been beneficial for some patients, helping to manage pain and improve mobility.
- Lifestyle Modifications: Making certain lifestyle changes can significantly impact the management of scoliosis:
- Weight Management: Maintaining a healthy weight can reduce stress on the spine.
- Posture Correction: Learning and practicing good posture can help alleviate pain and prevent the curvature from worsening.
- Regular Exercise: Activities like swimming or cycling can maintain flexibility and strength without putting excessive pressure on the spine.
Surgical Treatments
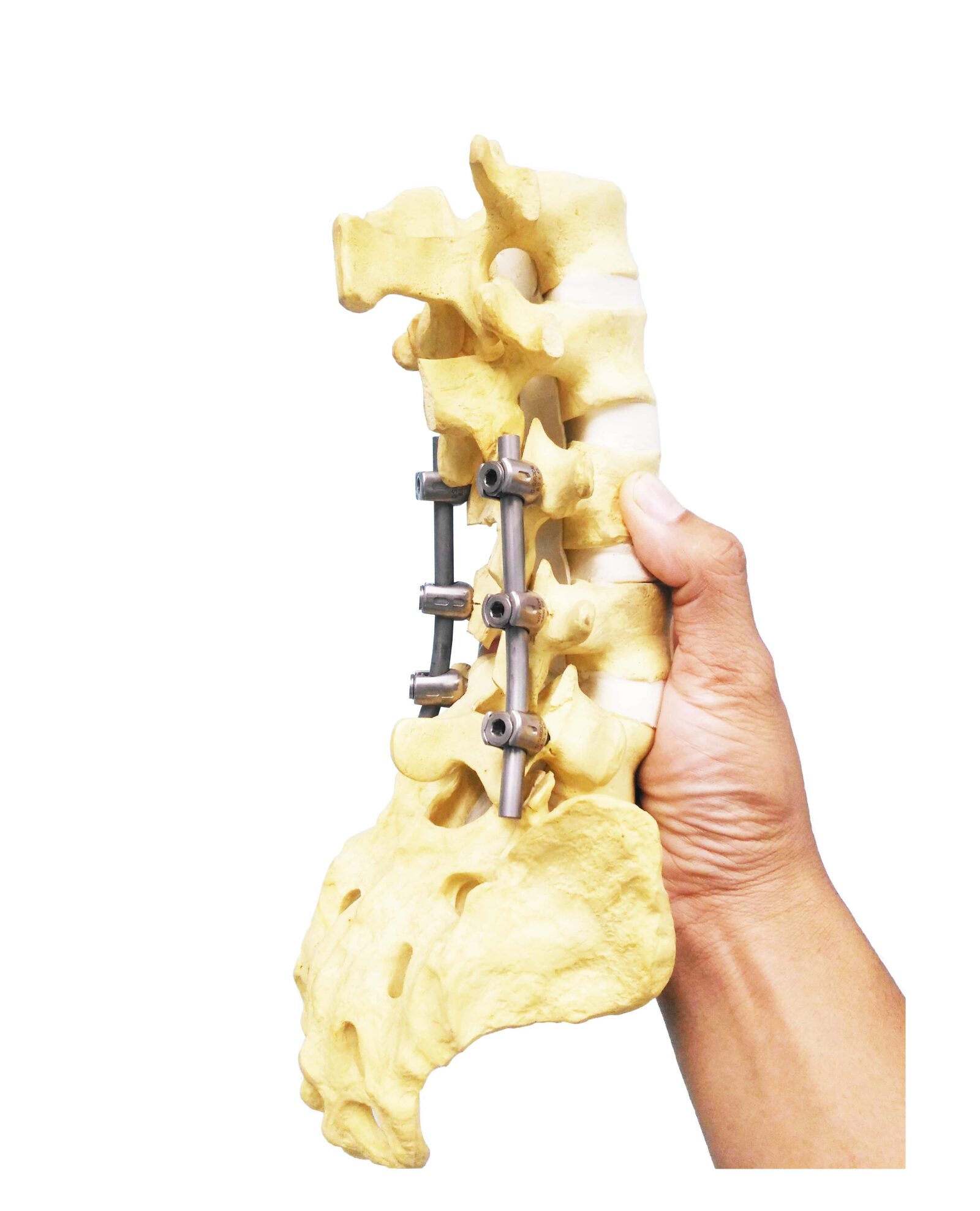
Surgery may be considered for adults whose curves are severe or progressing, or when non-surgical treatments fail to relieve disabling symptoms. The decision to proceed with surgery depends on several factors, including the severity of the curve, the presence of nerve compression, and overall health.
- Spinal Fusion: This is the most common surgical procedure for scoliosis in adults. It involves joining two or more vertebrae together permanently, using bone grafts and metal rods to stabilize the spine.
- Vertebral Body Tethering (VBT): VBT is a less invasive surgical option that involves placing screws in the vertebrae connected by a flexible cord, which helps to straighten the spine as it grows.
- Risks and Outcomes: Like all surgeries, spinal surgeries carry risks such as infection, blood loss, nerve damage, or complications related to anesthesia. The outcomes can vary widely, but many patients experience significant reductions in pain and improvements in their ability to perform daily activities.
The choice between non-surgical and surgical treatments depends on individual factors including age, severity of symptoms, curve progression, and personal preferences. Consultation with a spine specialist is crucial to determine the most appropriate treatment plan based on the specific circumstances of the individual.
Conclusion
In conclusion, managing adult scoliosis involves a multifaceted approach tailored to each individual’s specific condition and needs. From non-surgical options like physical therapy and pain management to surgical interventions for more severe cases, the goal is always to enhance quality of life, reduce pain, and improve functionality. Recognizing the symptoms early and consulting with healthcare professionals can lead to more effective management of the condition. As research continues and treatment technologies advance, the prospects for managing adult scoliosis effectively continue to improve, offering hope and improved outcomes for those affected by this complex spinal condition.










