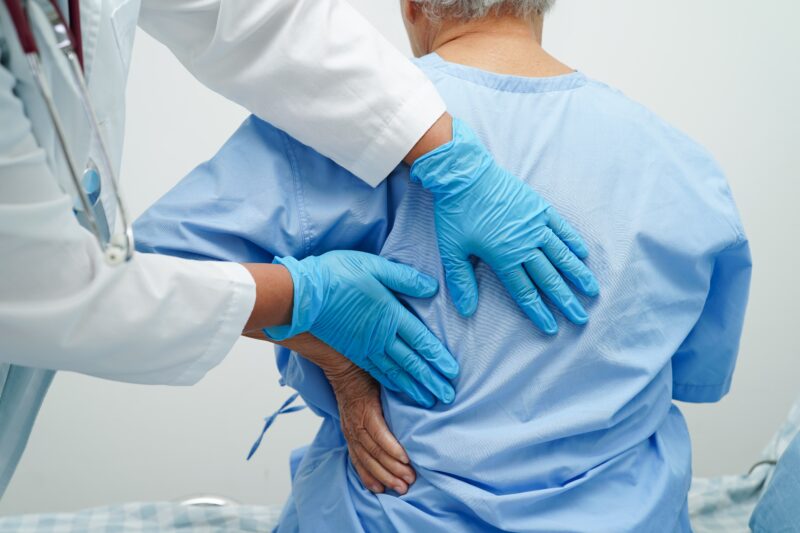
Failed Back Surgery Syndrome (FBSS) is a perplexing and often debilitating condition that affects a significant number of patients who undergo spinal surgery. As its name suggests, FBSS refers to the unfortunate circumstance where patients continue to experience pain or develop new pains following back surgery, indicating a less-than-successful outcome. Understanding FBSS is crucial for those considering spinal surgery or grappling with its aftereffects. Knowing how FBSS manifests, how it can be addressed, and most importantly, how patients can navigate their journey towards better health and wellbeing despite this complex syndrome.
#1 FBSS Can Have Many Causes
Failed Back Surgery Syndrome (FBSS) is a condition characterized by persistent or new pain following spinal surgery. Contrary to what the name might suggest, FBSS does not necessarily imply surgical failure; rather, it represents a situation where the intended outcome of pain relief and improved function is not achieved. The causes of FBSS are multifaceted and can include residual or recurrent disc herniation, postoperative scar tissue formation, persistent nerve compression or damage, spinal joint issues, and changes in spinal alignment or biomechanics. Additionally, surgeries might fail to address the underlying cause of the original pain, or new pain sources may develop. Factors such as patient health, surgical technique, and the complexity of the individual’s spinal condition all contribute to the risk of developing FBSS, making it a challenging condition both to predict and to manage effectively.
#2 Pain May Be Different Than Before
The symptoms of Failed Back Surgery Syndrome (FBSS) can be varied and complex, primarily manifesting as persistent or new pain following spinal surgery. Patients often experience chronic back or leg pain, which might be similar to or different from the pain they experienced pre-surgery. Other common symptoms include numbness, tingling sensations, and muscle weakness, which can significantly impact daily functioning and quality of life. Diagnosing FBSS is equally challenging, as it involves differentiating the syndrome from other potential causes of pain. A comprehensive approach is typically employed, encompassing a thorough review of the patient’s medical history, a detailed physical examination, and diagnostic imaging like MRI or CT scans to assess structural changes post-surgery. In some cases, nerve conduction studies may also be conducted to evaluate nerve damage. The process requires careful consideration by healthcare professionals to ensure accurate diagnosis and appropriate subsequent treatment.
#3 Treatment Options are Usually Multifaceted
Treatment options for Failed Back Surgery Syndrome (FBSS) are diverse and tailored to the individual’s specific symptoms and underlying causes. A multidisciplinary approach is often the most effective, combining physical therapy, medication management, and, in some cases, further surgical interventions. Physical therapy plays a crucial role in improving mobility and strength, while pain management may include both over-the-counter and prescription medications, including nerve pain treatments and muscle relaxants. Interventional therapies like nerve block injections or epidural steroid injections can also provide significant relief. For some patients, minimally invasive procedures or revision surgeries might be considered, although these are approached with caution due to the complexity of FBSS. In addition to these treatments, complementary therapies such as acupuncture, chiropractic care, and psychological support can be integral in managing chronic pain and improving overall quality of life. This comprehensive approach ensures that treatment is holistic, addressing both the physical and emotional aspects of living with FBSS.
#4 Physical Therapy Can Help
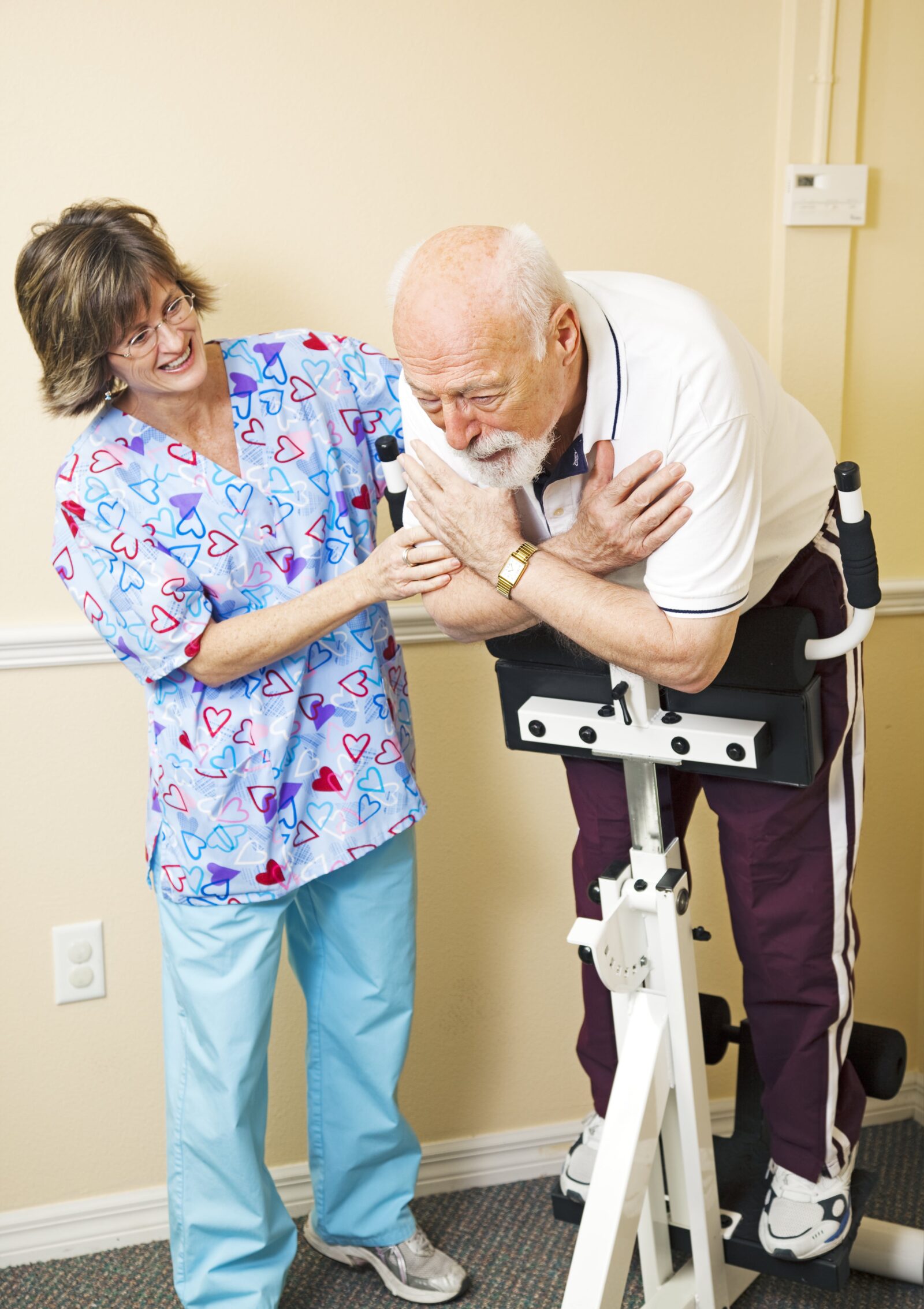
Physical therapy plays a pivotal role in the treatment and management of Failed Back Surgery Syndrome (FBSS). It is a cornerstone of non-invasive care, focusing on alleviating pain, improving mobility, and restoring function. Physical therapists tailor exercise programs to each patient’s specific needs, emphasizing core strengthening, flexibility, and stability exercises that support the spine. These exercises are designed not only to alleviate current discomfort but also to prevent future pain episodes. Physical therapy often includes manual therapy techniques, such as massage and mobilization, to improve movement in the spine and reduce muscle tension. Additionally, therapists may incorporate pain relief modalities like heat or cold therapy and electrical stimulation. An essential aspect of physical therapy for FBSS patients is education on proper body mechanics and ergonomic practices to protect the spine during daily activities. By combining these approaches, physical therapy aids in managing symptoms, enhancing quality of life, and potentially reducing the need for further surgical interventions.
#5 Psychological Impact Can Exacerbate Pain
The psychological impact of Failed Back Surgery Syndrome (FBSS) is profound and often an overlooked aspect of the condition. Living with chronic pain and the disappointment of an unsuccessful surgery can lead to significant emotional distress. Patients frequently experience feelings of frustration, anxiety, and depression, compounded by the limitations in mobility and daily activities. The chronic nature of the pain often disrupts sleep, exacerbates stress, and can lead to a sense of isolation or helplessness. This psychological toll can, in turn, intensify the perception of pain, creating a challenging cycle of physical discomfort and emotional suffering. Recognizing and addressing these mental health aspects is crucial in the overall management of FBSS. Psychological support, whether through counseling, cognitive-behavioral therapy, or support groups, is essential for helping patients cope with the emotional burden of the syndrome. Such support not only aids in improving mental well-being but can also have a positive effect on physical symptoms, leading to better overall outcomes.
#6 FBSS Can Be Prevented in Some Cases
Prevention strategies for Failed Back Surgery Syndrome (FBSS) are key in reducing the incidence and severity of this challenging condition. The cornerstone of prevention lies in ensuring accurate diagnosis and appropriate surgical indications before any spinal operation. This involves thorough diagnostic testing and imaging to correctly identify the source of spinal pain and determine if surgery is indeed the best option. Selecting the right surgical procedure and an experienced surgeon is also crucial, as is the use of minimally invasive techniques where appropriate, which can reduce tissue damage and postoperative complications. Patient education plays a vital role, too; understanding the surgery, realistic expectations, and post-operative care can significantly influence outcomes. Additionally, patients are encouraged to adopt a healthy lifestyle pre- and post-surgery, including maintaining a healthy weight, engaging in regular physical activity, and avoiding tobacco use, as these factors can affect spinal health and recovery. Adherence to post-operative care, including physical therapy and follow-up appointments, is essential in preventing complications that could lead to FBSS. By addressing these various factors, the risk of developing FBSS can be substantially mitigated.
#7 Long-Term Management Can Improve Symptoms
The long-term management of Failed Back Surgery Syndrome (FBSS) requires a comprehensive and adaptive approach, focusing on both alleviating symptoms and improving the quality of life for patients. Central to this management is ongoing pain control, which may involve a combination of medications, physical therapy, and possibly interventional pain procedures like nerve blocks or radiofrequency ablations. Regular physical therapy is essential to maintain mobility, strengthen the back and core muscles, and reduce the risk of further injury. Lifestyle modifications play a significant role; patients may need to adjust their daily activities, adopt ergonomic practices at work, and engage in regular, low-impact exercises like walking, swimming, or yoga to keep the body active without exacerbating pain. Nutritional support and maintaining a healthy weight can also help manage symptoms and improve overall health. Psychological support, including therapy and support groups, can be crucial in helping patients cope with the chronic nature of their pain and the emotional toll it can take. Regular follow-up with healthcare providers is important to monitor the condition and adjust treatment plans as needed. This long-term, multidisciplinary approach aims not just to manage pain, but also to empower patients with FBSS to lead fulfilling and active lives.
Conclusion
In conclusion, Failed Back Surgery Syndrome (FBSS) presents a complex and multifaceted challenge, both to patients and healthcare professionals. Understanding its varied causes, symptoms, and the necessity for a multidisciplinary treatment approach is crucial for effective management. While physical therapy and pain management are fundamental in addressing the physical aspects of FBSS, acknowledging and treating the psychological impact is equally important for a holistic approach to patient care. Prevention strategies, focusing on accurate diagnosis and appropriate surgical decisions, play a key role in reducing the incidence of FBSS. Long-term management, involving a combination of medical, physical, and psychological support, is essential for improving quality of life and functionality in patients. Ultimately, navigating the intricacies of FBSS requires patience, persistence, and a collaborative effort between patients and their healthcare teams to achieve the best possible outcomes.