Osteoporosis, often dubbed the “silent disease,” is a condition that sneaks up on millions worldwide, weakening their bones and leaving them vulnerable to fractures. While it can affect any bone in the body, its impact on the spine is particularly profound and, at times, devastating. The spine, a central pillar of our skeletal system, plays a pivotal role in our mobility, posture, and overall well-being. When compromised by osteoporosis, the repercussions can be both physically and emotionally debilitating. In this blog, we’ll delve deep into the intricate relationship between osteoporosis and spinal health.
The Science Behind Bone Density Loss
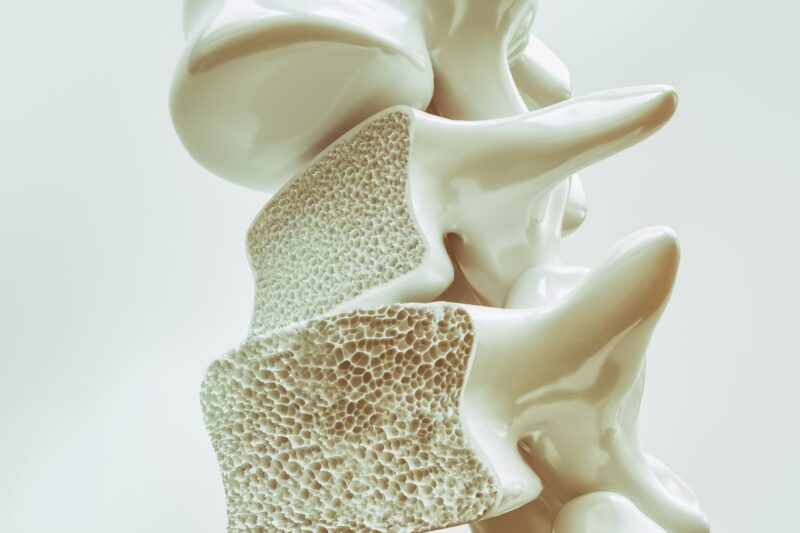
Osteoporosis is a bone disease characterized by a decrease in bone density and strength, leading to fragile bones that are more prone to fractures. The term “osteoporosis” is derived from Greek words meaning “porous bone.” When viewed under a microscope, healthy bone tissue appears as a honeycomb. However, in osteoporosis, the holes and spaces in this honeycomb structure become larger, indicating a loss of bone mass and minerals.
At its core, osteoporosis is a result of an imbalance in the bone remodeling process. Our bones are in a constant state of renewal, with old bone being broken down and new bone being formed. However, as we age or due to certain medical conditions and medications, the balance tips. The body may start to remove more bone than it replaces, leading to a decrease in bone density.
How Osteoporosis Affects the Spine
Osteoporosis has a significant impact on the spine, given that the vertebral bones are among the most common sites affected by this condition. Here’s how osteoporosis affects the spine:
Vertebral Compression Fractures:
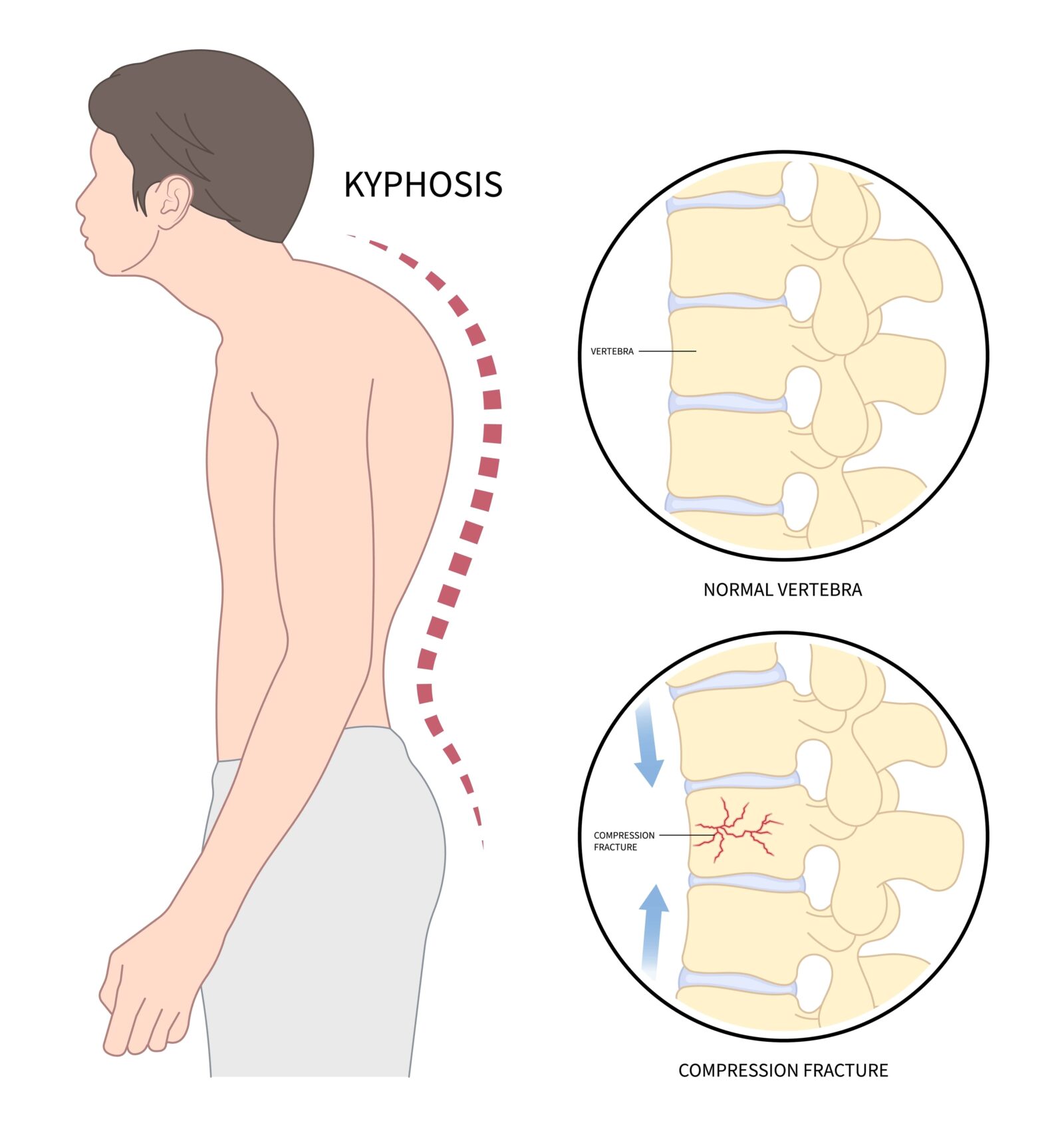
One of the most direct and severe consequences of osteoporosis on the spine is vertebral compression fractures. These fractures occur when the bony block or vertebral body in the spine collapses, which can lead to severe pain, deformity, and loss of height. These fractures can be caused by simple daily activities, such as lifting a heavy object, or even by minor events like coughing or sneezing in severe cases.
Kyphosis (Dowager’s Hump):
Multiple vertebral compression fractures can result in a forward curvature of the spine, known as kyphosis or more commonly referred to as a “dowager’s hump.” This curvature can lead to a hunched or stooped posture, which can be both painful and debilitating.
Chronic Pain:
Even without a noticeable fracture, osteoporosis can cause chronic back pain. The pain can be due to microfractures, changes in the architecture of the bones, or muscle strain resulting from changes in posture.
Decreased Mobility:
The pain and structural changes associated with osteoporosis can limit mobility. This decreased mobility can further contribute to bone loss due to reduced physical activity, creating a vicious cycle.
Height Loss:
Over time, repeated vertebral fractures can lead to a noticeable loss of height. This height loss is not just cosmetic; it can also affect lung capacity and digestive function.
Nerve Compression:
In some cases, the changes in the vertebral structure can lead to nerve compression, causing symptoms like numbness, tingling, or even weakness in the limbs.
Reduced Quality of Life:
The combined effects of pain, decreased mobility, and potential deformity can significantly impact an individual’s quality of life. It can lead to reduced independence, increased isolation, and even depression.
Signs and Symptoms of Spinal Osteoporosis
While osteoporosis is often silent until a fracture occurs, there are some signs that might indicate its presence:
- Chronic back pain, especially if it’s sharp and sudden.
- Loss of height over time.
- A stooped posture.
- Frequent fractures in other parts of the body.
It’s essential to consult with a healthcare professional if you notice any of these symptoms. Early detection can lead to more effective management and treatment.
Prevention and Treatment
Preventing and treating spinal osteoporosis involves a combination of lifestyle changes, medications, and interventions. The goal is to maintain or increase bone density, reduce the risk of fractures, and manage any associated pain or complications. Here’s a comprehensive look at the prevention and treatment of spinal osteoporosis:
Prevention:
- Dietary Calcium and Vitamin D: Ensure adequate intake of calcium and vitamin D, which are essential for bone health. Dairy products, green leafy vegetables, fortified foods, and supplements can be good sources.
- Regular Exercise: Weight-bearing exercises like walking, jogging, and strength training can help maintain bone density. Balance exercises can also reduce the risk of falls, which can lead to fractures.
- Avoid Smoking and Limit Alcohol: Smoking is detrimental to bone health, and excessive alcohol can increase the risk of falls and fractures.
- Bone Density Testing: Regular bone density tests (like DEXA scans) can help in early detection of osteoporosis and assess fracture risk.
- Limit Caffeine: Excessive caffeine consumption can interfere with calcium absorption.
- Fall Prevention: Make home modifications to reduce the risk of falls. This includes securing rugs, installing grab bars, and improving lighting.
Treatment:

- Bisphosphonates: These are the most commonly prescribed medications for osteoporosis. They slow down the process of bone resorption, helping to maintain or increase bone density. Examples include alendronate (Fosamax), risedronate (Actonel), and zoledronic acid (Reclast).
- Hormone Replacement Therapy (HRT): For postmenopausal women, HRT can help maintain bone density. However, it comes with potential risks, so it’s essential to discuss the pros and cons with a healthcare provider.
- Selective Estrogen Receptor Modulators (SERMs): Drugs like raloxifene (Evista) mimic estrogen’s beneficial effects on bone density without some of the risks associated with HRT.
- Parathyroid Hormone (PTH) Therapy: Teriparatide (Forteo) is a form of PTH that stimulates new bone formation. It’s used for individuals with severe osteoporosis.
- Monoclonal Antibodies: Denosumab (Prolia) is a biologic medication that can help increase bone density and strength.
- Pain Management: Over-the-counter pain relievers, prescription medications, and physical therapy can help manage pain associated with fractures or spinal deformities.
- Surgical Interventions: In cases of severe vertebral fractures, procedures like vertebroplasty or kyphoplasty can be considered. These involve injecting bone cement into the fractured vertebra to stabilize it.
- Bracing: In some cases, wearing a brace can help support the spine, reduce pain, and prevent further curvature.
- Calcitonin: This hormone, available as a nasal spray or injection, can help regulate bone metabolism and provide pain relief after a vertebral fracture.
Regular check-ups and consultations with healthcare providers are crucial for individuals at risk of or diagnosed with spinal osteoporosis. Personalized treatment plans, regular monitoring, and proactive measures can help manage the condition effectively and improve the quality of life.
In Conclusion
In the face of the silent threat that is osteoporosis, awareness and proactive intervention are our strongest allies. Spinal osteoporosis, in particular, can have profound implications on an individual’s quality of life, from chronic pain to mobility challenges. However, with the right preventive measures, timely diagnosis, and tailored treatments, it’s possible to combat the progression of this condition. By prioritizing bone health, embracing a balanced lifestyle, and seeking regular medical guidance, we can safeguard our spine’s integrity and continue to lead active, fulfilling lives.