Spinal conditions, ranging from acute injuries to chronic diseases, can have a profound impact on an individual’s quality of life. Managing these conditions effectively is crucial, and diagnostic imaging plays a pivotal role in this process. In this blog, we’ll explore the significance of diagnostic imaging in the diagnosis, treatment, and management of spinal conditions.
Understanding Spinal Conditions
To appreciate the significance of diagnostic imaging in managing spinal conditions, it’s essential to understand basic spinal anatomy and the common conditions that affect this vital part of the human body.
Spinal Anatomy
The human spine is a remarkable structure, designed for both flexibility and strength. It extends from the base of the skull to the tailbone and is composed of three main segments:
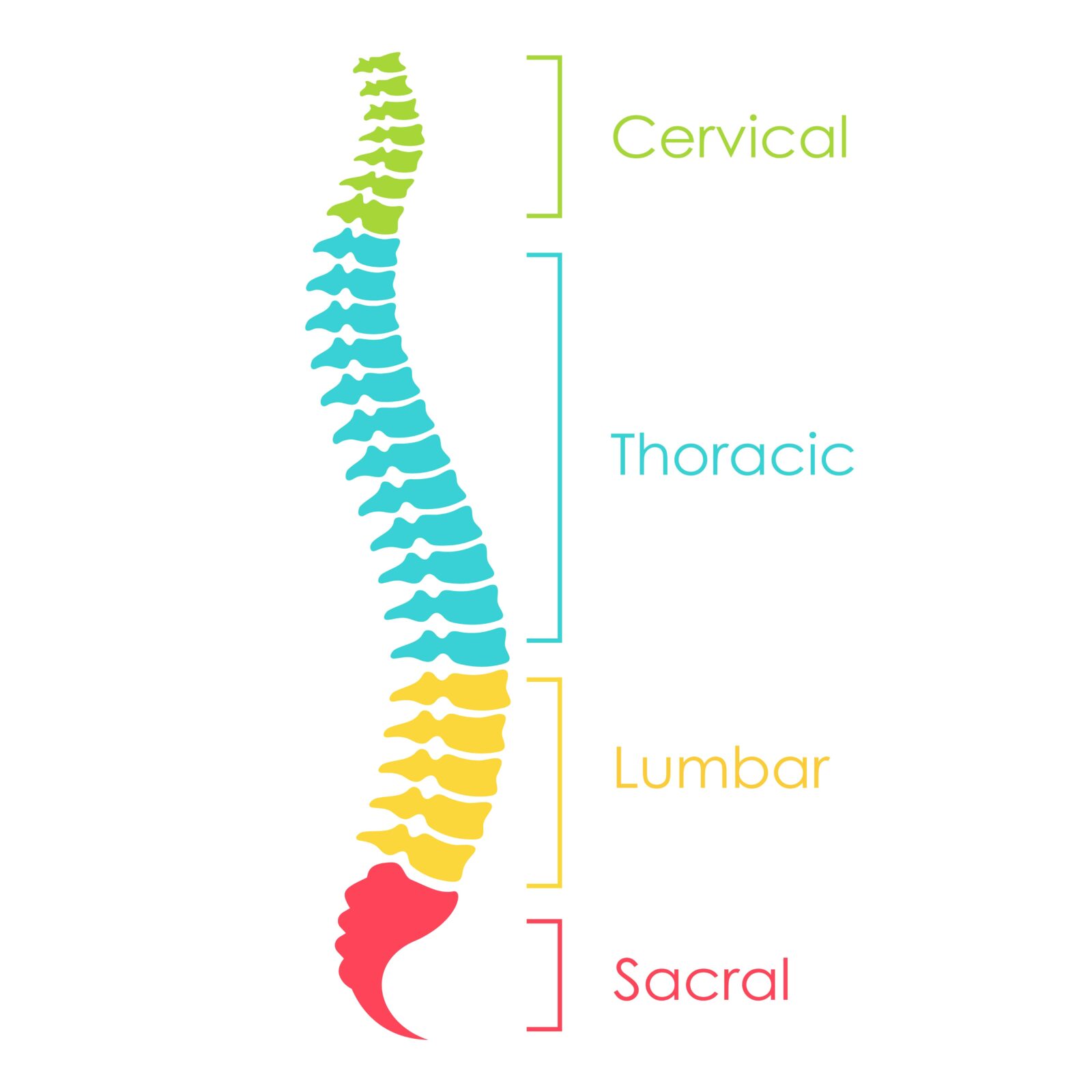
- Cervical Spine: This is the upper part of the spine, consisting of seven vertebrae (C1-C7) in the neck. It supports the head and allows for a wide range of head movements.
- Thoracic Spine: Comprising twelve vertebrae (T1-T12), the thoracic spine is located in the upper and mid-back. It attaches to the ribcage and plays a crucial role in supporting the upper body.
- Lumbar Spine: The lower back, consisting of five larger vertebrae (L1-L5), bears the weight of the torso, making it a common area for pain and injury.
Between the vertebrae are intervertebral discs, which act as shock absorbers and provide flexibility to the spine. The spinal cord runs through the central canal of the vertebrae, transmitting messages between the brain and the body.
Common Spinal Conditions
Various conditions can affect the spine, leading to pain, discomfort, and mobility issues. Some of the common spinal conditions include:
- Herniated Disc: This occurs when the soft inner material of an intervertebral disc protrudes through the outer layer, often compressing nearby nerves and causing pain.
- Degenerative Disc Disease: This age-related condition involves the gradual deterioration of the intervertebral discs, which can lead to pain and reduced mobility.
- Spinal Stenosis: This condition involves the narrowing of the spinal canal, which can compress the spinal cord and nerves, causing pain, numbness, or weakness.
- Scoliosis: A condition characterized by an abnormal sideways curvature of the spine, which can lead to discomfort and various physical complications.
- Osteoarthritis: This is a degenerative joint disease that can affect the spine’s joints, leading to stiffness, pain, and reduced movement.
- Spinal Fractures and Trauma: Accidents or falls can lead to fractures or other injuries to the spine, requiring immediate medical attention.
Understanding these conditions and their impact on spinal anatomy underscores the importance of accurate diagnosis and effective management, where diagnostic imaging plays a crucial role. By visualizing the intricate structures of the spine and identifying abnormalities, healthcare providers can tailor treatment plans to address specific spinal conditions effectively.
The Role of Diagnostic Imaging
Early and Accurate Diagnosis
Early diagnosis is critical in managing spinal conditions. Diagnostic imaging techniques such as X-rays, Magnetic Resonance Imaging (MRI), Computed Tomography (CT) scans, and ultrasound play a vital role in this. They provide detailed images of the spine’s anatomy, helping healthcare providers to identify the exact cause and location of the problem. Imaging not only detects the presence of a condition but also helps in assessing its severity. For instance, an MRI can show the extent of a disc herniation and its impact on nearby nerves.
- X-rays are often the first step in spinal imaging. They are excellent for viewing bone structures, identifying fractures, and looking for spinal misalignments.
- MRI offers detailed images of soft tissues, including discs, nerves, and ligaments. It’s particularly useful in diagnosing conditions like herniated discs, spinal cord injuries, and tumors.
- CT scans provide detailed images of both bone and soft tissues. They are often used when MRI is contraindicated, such as in patients with implanted medical devices.
- Ultrasound is less commonly used for spinal conditions but can be helpful in assessing soft tissue abnormalities near the spine.
Guiding Treatment
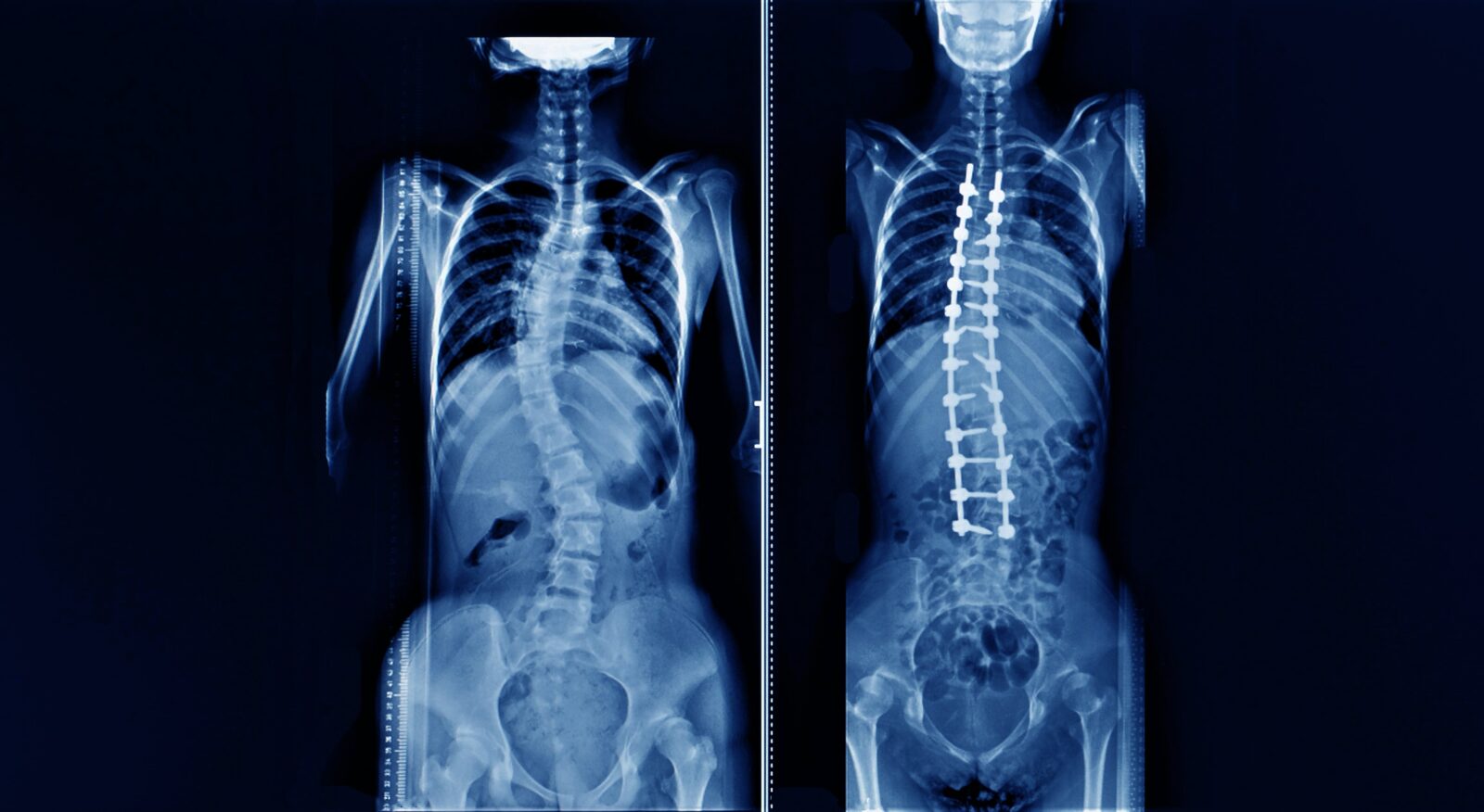
Diagnostic imaging not only aids in diagnosis but also guides treatment. By offering detailed visualizations of the spine, these technologies allow healthcare professionals to tailor treatment plans specifically to the patient’s unique condition. For instance, an MRI can reveal the exact location and severity of a herniated disc, enabling a surgeon to strategize a targeted surgical approach. Similarly, CT scans can be instrumental in detecting bone abnormalities or spinal fractures, influencing decisions about surgical intervention versus conservative management. In cases of spinal deformities like scoliosis, imaging aids in determining the extent of curvature and guides the planning of corrective surgeries or bracing treatments. Beyond aiding in initial treatment decisions, diagnostic imaging also plays a vital role in monitoring the progress of ongoing treatments, such as assessing the healing after spinal surgery or evaluating the effectiveness of non-surgical interventions like physical therapy. By providing a clear and precise picture of the spine’s condition at every stage, diagnostic imaging ensures that each patient receives the most appropriate, effective, and personalized treatment plan.
Interventional Procedures
Diagnostic imaging is indispensable in the realm of interventional procedures for spinal conditions, offering real-time guidance and increased precision. Techniques such as fluoroscopy, a live X-ray method, play a pivotal role in procedures like epidural steroid injections, nerve blocks, and the placement of spinal cord stimulators. These imaging modalities allow physicians to visualize the spine’s anatomy in great detail and in real-time, ensuring that interventions are accurately targeted. For instance, during an epidural injection, fluoroscopy guides the needle to the exact location in the spine where medication is needed, minimizing the risk of damage to surrounding tissues and maximizing therapeutic effectiveness. Similarly, in the placement of spinal cord stimulators, imaging ensures the electrodes are positioned precisely to provide pain relief. This real-time visualization not only enhances the safety and efficacy of the procedures but also reduces the risk of complications, leading to better outcomes for patients with spinal ailments. Diagnostic imaging, thus, transforms intricate spinal interventions into safer, more precise, and more effective treatments.
Monitoring Rehabilitation
Post-treatment, imaging is crucial in monitoring the recovery and rehabilitation process. It helps in assessing the healing of spinal injuries or the success of surgical interventions. For example, a follow-up MRI can show whether a surgical intervention successfully alleviated the issue at hand. For patients undergoing physical therapy, periodic imaging can provide feedback on the effectiveness of the treatment plan. In chronic conditions like osteoarthritis or degenerative disc disease, periodic imaging can monitor the progression of the disease and the effectiveness of ongoing treatments.
Preventing Complications
Diagnostic imaging plays a vital role in the prevention of complications in spinal conditions. By providing detailed and accurate images of the spine, these technologies enable early detection of potential issues that might otherwise go unnoticed until they become more severe. For instance, regular MRI or CT scans can identify subtle changes or worsening of a condition like spinal stenosis or a slowly progressing spinal tumor, allowing for timely intervention. This early intervention can prevent the development of more serious complications such as nerve damage, chronic pain, or even paralysis. Furthermore, in post-surgical patients, imaging can detect complications like infections, hardware malfunctions, or issues with spinal alignment before they manifest as serious clinical problems. By allowing for prompt and appropriate responses to these findings, diagnostic imaging plays a crucial role in maintaining the health and function of the spine, reducing the risk of long-term disability, and improving overall patient outcomes in spinal care.
Conclusion
In summary, diagnostic imaging is a cornerstone in the management of spinal conditions. It offers a window into the intricate structures of the spine, enabling healthcare professionals to diagnose accurately, plan and execute treatment effectively, monitor progress, and adjust care plans as needed for optimal patient outcomes.
Remember, if you’re experiencing back pain or other symptoms suggestive of a spinal condition, consult a healthcare professional. They can guide you on the appropriate diagnostic imaging needed for your condition.