Spinal discs play a crucial role in our vertebral column, providing support, flexibility, and shock absorption. However, various conditions can affect these discs, leading to discomfort and reduced quality of life. In this comprehensive guide, we will delve into four common spinal disc conditions: degenerative disc disease, disc protrusion, herniated disc, and Schmorl’s hernia.
Anatomy of a Healthy Spinal Disc: Understanding the Structure and Function
The spinal disc is a remarkable structure that plays a vital role in maintaining the health and flexibility of our spine. Composed of fibrocartilage, these intervertebral discs are located between each pair of adjacent vertebrae, acting as shock absorbers and allowing for smooth movement. Understanding the anatomy of a healthy spinal disc is essential to appreciate its function and the potential impact of various disc-related conditions.
Structure of a Spinal Disc
A healthy spinal disc consists of two main components:
- Annulus Fibrosus: The annulus fibrosus is the outer layer of the disc and provides strength and stability. It is made up of multiple layers of collagen fibers arranged in a crisscross pattern. These fibers are densely packed and arranged in different angles, giving the annulus fibrosus its resilience and flexibility. The annulus fibrosus also helps contain the inner nucleus pulposus.
- Nucleus Pulposus: The nucleus pulposus is the gel-like center of the disc. It is composed mainly of water, proteoglycans, and a network of collagen fibers. This composition enables the nucleus pulposus to absorb and distribute pressure evenly throughout the disc, acting as a shock absorber during various movements and activities. The high water content provides the disc with its ability to compress and expand.
Function of a Spinal Disc
A healthy spinal disc serves several crucial functions:
- Shock Absorption: The intervertebral discs act as shock absorbers, cushioning the spine during daily activities such as walking, running, or lifting heavy objects. The gel-like nucleus pulposus absorbs external forces and distributes them evenly across the disc, minimizing the impact on the vertebrae and preventing damage.
- Flexibility and Mobility: The structure of the spinal disc allows for flexibility and mobility in the spine. The arrangement of the annulus fibrosus and its fibrous layers provides stability and prevents excessive movement between the vertebrae, while still allowing for a wide range of motion.
- Load Distribution: The spinal discs help distribute the weight and load evenly across the spinal column. This distribution prevents excessive stress on individual vertebrae, ensuring balanced support and minimizing the risk of structural damage.
- Nutrition Supply: Unlike other structures in the body, spinal discs do not have a direct blood supply. Instead, they receive nutrients and oxygen through a process called imbibition. Imbibition occurs when pressure is applied to the disc, forcing water and essential nutrients into the disc. This process is facilitated by movement, which is why regular exercise and proper spinal alignment are crucial for maintaining a healthy disc.
Common Spinal Disc Conditions
Degenerative Disc Disease
Degenerative disc disease (DDD) is a condition that affects the intervertebral discs, the cushion-like structures located between the vertebrae in the spine. As the name suggests, DDD involves the gradual degeneration and deterioration of these discs over time. The condition typically starts with age-related changes but can also be influenced by genetics, lifestyle factors, and injuries. The degeneration of the spinal discs in DDD involves the loss of disc height and water content, leading to decreased flexibility and shock absorption. Structural changes, such as tears or cracks in the outer layer of the discs, can occur, weakening their integrity. The body may respond by forming bone spurs around the affected area, further contributing to stiffness and potential nerve compression. These changes can result in chronic back pain, stiffness, limited mobility, and, in some cases, radiating pain, numbness, or weakness due to nerve compression. While degenerative disc disease is not reversible, various treatment options aim to manage symptoms, improve functionality, and slow down the progression of the condition.
Disc Protrusion (Bulging Disc)
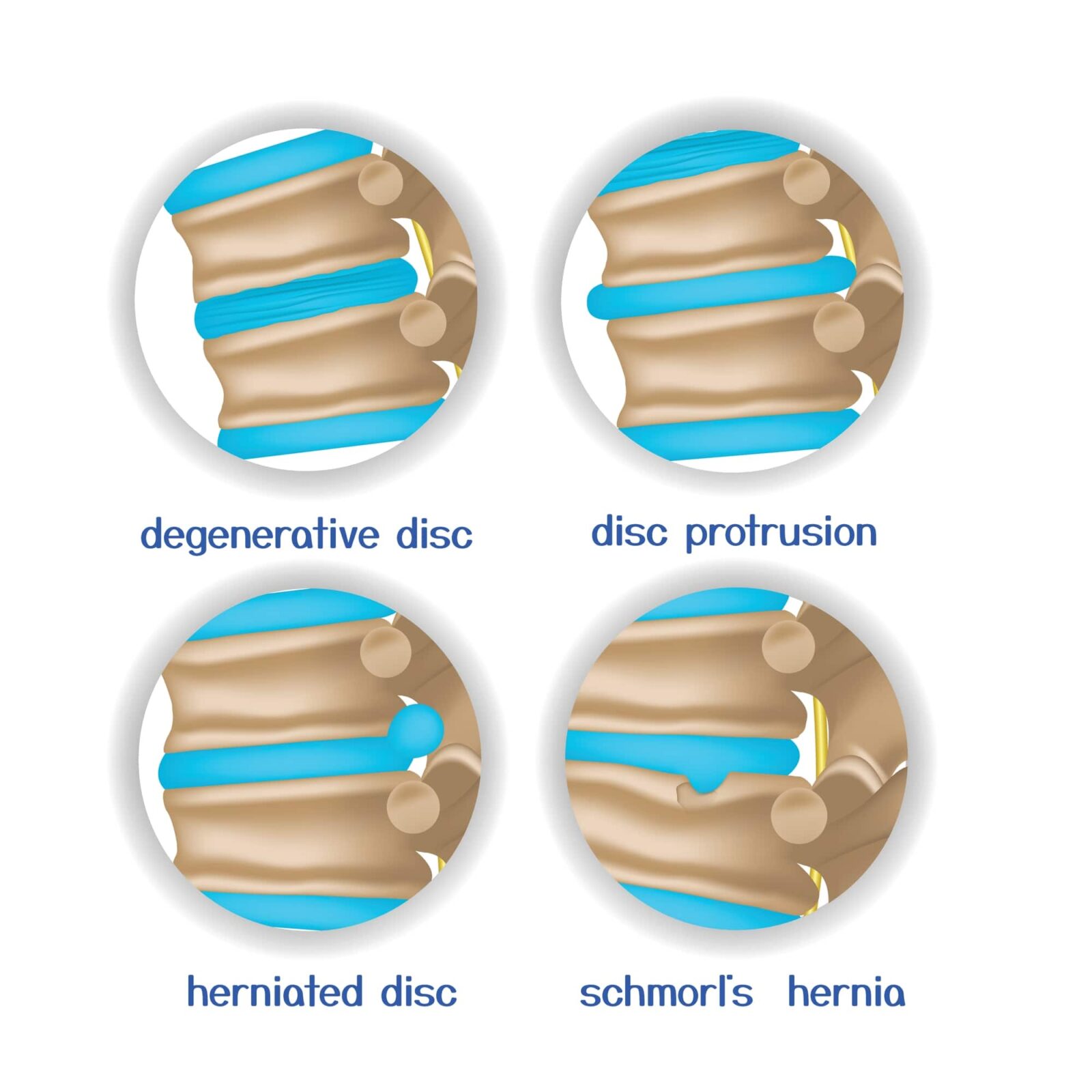
Disc protrusion is a condition in which a spinal disc bulges abnormally, potentially impacting the surrounding structures and affecting the overall function of the spine. Disc protrusion is also sometimes known as a bulging disc. It can occur due to factors such as trauma, repetitive motion, or poor posture. When a disc protrudes, its outer layer weakens or develops small tears, causing the gel-like inner material to push against it. This bulging disc can lead to localized pain and discomfort, as well as radiating pain, tingling, or muscle weakness if it compresses nearby spinal nerves. The protrusion can affect the overall function of the spine by limiting its range of motion and causing instability. It may also disrupt the alignment of the vertebrae, leading to issues with posture and movement. Proper diagnosis through physical examinations and imaging tests is crucial to determine the extent of the protrusion and guide appropriate treatment. Non-surgical approaches such as physical therapy, pain management, and ergonomic adjustments are often employed to alleviate symptoms and improve spinal function. In severe cases, surgical interventions may be necessary to address the disc protrusion and restore spinal stability. Adopting good posture, avoiding excessive strain on the spine, and maintaining a healthy lifestyle can help prevent disc protrusion and promote the overall health and function of the spine.
Herniated Disc
Disc herniation, also known as a slipped or ruptured disc, occurs when the inner core of a spinal disc pushes through a weakened or damaged area of the outer layer. It is important to note that a herniated disc is different from a bulging disc. This condition can result from trauma, repetitive stress, or natural wear and tear. When a disc herniates, it can cause various effects on the spinal discs. The herniation disrupts the disc’s structure and integrity, compromising its ability to function properly. This can lead to localized pain, as well as radiating pain, tingling, numbness, or muscle weakness if the herniated disc compresses nearby spinal nerves. The herniation can also cause inflammation, further contributing to discomfort and irritation. The overall function of the spinal discs is affected as the herniated disc can reduce flexibility, stability, and shock absorption in the spine. Proper diagnosis through physical examinations and imaging tests is essential to identify the herniated disc and guide appropriate treatment. Non-surgical interventions like rest, medication, physical therapy, and lifestyle modifications are often recommended to manage symptoms and support healing. In severe cases or when conservative measures fail, surgical procedures may be considered to address the herniated disc and alleviate nerve compression. Engaging in regular exercise, maintaining proper body mechanics, and avoiding excessive strain on the spine are essential for preventing disc herniation and promoting spinal disc health.
Schmorl’s Hernia
Schmorl’s hernia, also known as vertebral endplate herniation, is a condition in which the nucleus pulposus of a spinal disc protrudes through the vertebral endplate and into the vertebral body. It can be caused by trauma, genetic factors, or excessive loading. Schmorl’s hernia typically affects the thoracic and lumbar spine but can occur in other regions as well. This herniation can lead to various effects on the spinal discs. The herniated nucleus pulposus can cause localized pain and discomfort in the affected area. It may also disrupt the structural integrity of the disc and compromise its ability to provide shock absorption and support. While Schmorl’s hernia often remains asymptomatic, it can occasionally lead to complications such as inflammation, nerve compression, or bone changes. Diagnosis is usually made through imaging techniques like X-rays or MRI scans. Treatment for Schmorl’s hernia typically involves pain management techniques, physical therapy, and lifestyle modifications to reduce symptoms and prevent further complications. Surgical interventions are less common but may be considered for severe cases. Maintaining a healthy weight, practicing good posture, and avoiding excessive spinal loading are important in reducing the risk of Schmorl’s hernia and supporting overall spinal disc health.
In Conclusion
Understanding the four common conditions affecting spinal discs is essential for maintaining spinal health and seeking timely medical intervention when necessary. Degenerative disc disease, disc protrusion, herniated disc, and Schmorl’s hernia can cause significant discomfort and impact our daily lives. By recognizing the symptoms, seeking proper diagnosis, and following recommended treatment options, individuals can effectively manage these conditions and reduce their impact on overall well-being. Prioritizing spinal health through preventive measures such as regular exercise, maintaining proper posture, and avoiding excessive strain on the spine is crucial in preserving a healthy spine for years to come. Remember, early detection and appropriate treatment are key to ensuring a pain-free and active lifestyle.