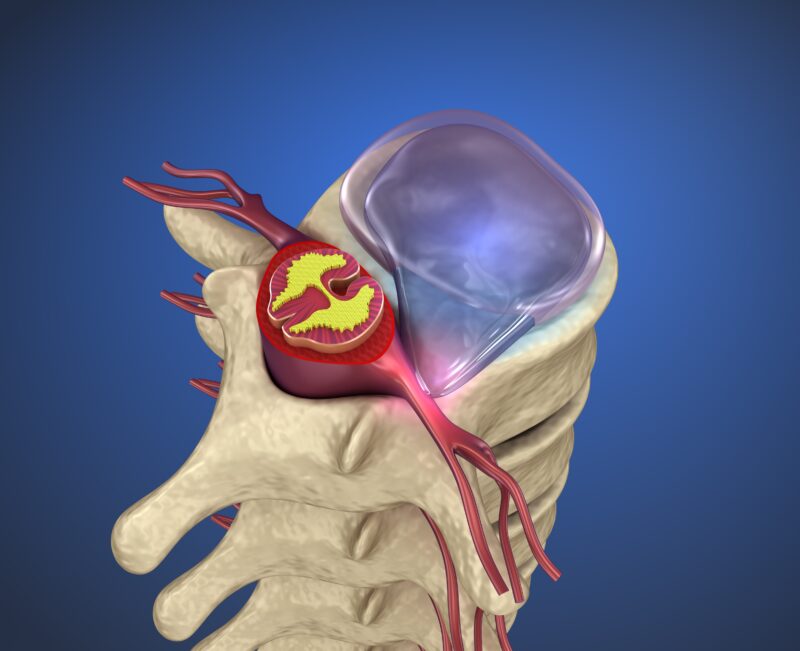
A herniated disc, often referred to as a slipped or ruptured disc, is a prevalent yet frequently misunderstood condition that affects the spine. In this blog, we’ll delve deep into the causes, symptoms, and various treatment options for herniated discs to demystify this complex spinal disorder. Understanding the anatomy of the spine, the mechanics behind disc deterioration, and the resulting symptoms is crucial for both patients and caretakers. By exploring how herniated discs can impact different regions of the spine and the potential consequences of untreated cases, we aim to provide valuable insights that can aid in managing and potentially alleviating this painful condition. Whether you’re suffering from a herniated disc or just interested in spine health, this guide will equip you with the knowledge needed to navigate the challenges associated with this disorder.
In This Blog:
- What is a Herniated Disc?
- Causes of Herniated Discs
- Symptoms of Herniated Discs
- Diagnosing Herniated Discs
- Treatment Options for Herniated Discs
What is a Herniated Disc?

A herniated disc occurs when the soft cushioning material between the vertebrae, known as the disc, pushes out through a tear in its tough exterior casing. This condition can lead to discomfort and disability, particularly when the herniated material compresses the nearby spinal nerves. The spine is composed of three main segments: the cervical (neck), thoracic (middle back), and lumbar (lower back) regions. Herniations most commonly occur in the lumbar region due to its high mobility and load-bearing function, with the cervical region being the second most common site.
There are several types of herniated discs based on the nature of the disc material’s displacement:
- Protrusion: The disc bulges without rupturing the outer layer.
- Extrusion: The disc material breaks through the outer layer but remains connected to the disc.
- Sequestration: Pieces of the disc material separate entirely from the disc.
Understanding these types can help tailor treatment approaches and anticipate potential complications.
Causes of Herniated Discs
Herniated discs are primarily caused by age-related wear and tear called disc degeneration. As we age, our spinal discs lose some of their water content, which makes them less flexible and more prone to tearing or rupturing with even a minor strain or twist. However, other factors can also contribute to the development of herniated discs:
- Physical strain and injury: Activities that involve repetitive lifting, pulling, bending, or twisting can increase the risk of a herniated disc. Sudden heavy lifting or a traumatic injury to the spine can cause acute herniations.
- Lifestyle factors: Obesity increases the stress on the discs in your lower back. Smoking may reduce oxygen supply to the disc, causing more rapid degeneration. A sedentary lifestyle may also predispose individuals to disc health problems.
- Genetic predisposition: There is some evidence suggesting that genetic factors might influence the susceptibility to developing disc degeneration and herniations.
Understanding these causes can help in both preventing herniated discs and managing them more effectively if they occur.
Symptoms of Herniated Discs
The symptoms of a herniated disc vary widely depending on the location of the herniation and whether the disc is pressing on a nerve. They can range from little to no pain if the disc is not pressing on a nerve, to severe, debilitating pain if nerve involvement occurs. Common symptoms include:
- Pain: This can be sharp or burning in nature and is typically felt on one side of the body. If the herniated disc is in the lumbar region, you might experience pain in the buttocks, thigh, and calf. A herniated disc in the cervical area can cause pain in the shoulders and arms.
- Numbness or tingling: People with a herniated disc often experience these sensations in the body part served by the affected nerves.
- Weakness: Muscles served by the affected nerves might weaken. This can cause stumbling or impair your ability to hold or lift items.
Complications can arise if a herniated disc is left untreated. For example, severe nerve compression can lead to permanent damage, and in cases involving compression of the spinal cord or cauda equina (the bundle of spinal nerves at the end of the spinal cord), it can be a medical emergency requiring immediate intervention.
By understanding the symptoms and the underlying causes, individuals can seek timely medical attention, potentially preventing the progression of symptoms and improving the overall quality of life.
Diagnosing Herniated Discs
Diagnosing a herniated disc accurately is crucial for effective management and treatment. The diagnostic process typically begins with a comprehensive physical examination where a healthcare provider evaluates the patient’s medical history and conducts a series of physical tests. These tests assess the patient’s reflexes, muscle strength, walking ability, and the ability to feel light touches, pinpricks, or vibration. In many cases, the location of the pain and the nature of the symptoms can give preliminary clues about the location of the herniated disc.
Following the physical examination, imaging tests are often necessary to confirm the diagnosis and pinpoint the exact location and severity of the herniation:
- MRI (Magnetic Resonance Imaging): This is the most frequently used imaging test for diagnosing herniated discs. It provides detailed images of the body’s soft tissues, including the condition of the discs and nerves.
- CT Scan (Computed Tomography): A CT scan can be used if MRI is not available, or in addition to MRI, providing a different form of imaging that can be useful in certain cases.
- X-rays: While X-rays can’t detect herniated discs, they can rule out other causes of back pain such as fractures, tumors, or spinal alignment problems.
In some instances, doctors might recommend nerve tests to detect nerve damage and determine its severity:
- Electromyography (EMG): This test measures the electrical impulses along nerve roots, peripheral nerves, and muscle tissue. This can indicate whether nerve compression caused by a herniated disc is also causing nerve damage.
- Nerve Conduction Studies (NCS): This test measures how well and how fast the nerves can send electrical signals. Nerve conduction testing can identify nerve damage and the area that is affected.
Treatment Options for Herniated Discs
Once a herniated disc has been diagnosed, treatment options range from conservative therapies to surgery, depending on the severity of the symptoms and the specific needs of the patient.
Non-surgical treatments:
- Medications: Over-the-counter pain relievers such as ibuprofen or naproxen can alleviate mild to moderate pain. In more severe cases, doctors may prescribe narcotics or muscle relaxants for a short period to relieve acute pain. Additionally, nerve pain medications, such as gabapentin or pregabalin, are used to treat pain associated with nerve damage.
- Physical Therapy: Physical therapists can teach exercises that strengthen the muscles supporting the spine, improve spine flexibility, and increase range of motion. Correct posture and body mechanics taught in physical therapy can also help relieve symptoms.
- Lifestyle Modifications: Weight management, quitting smoking, and adopting a physically active lifestyle can help reduce the risk of further disc injury.
Surgical treatments:
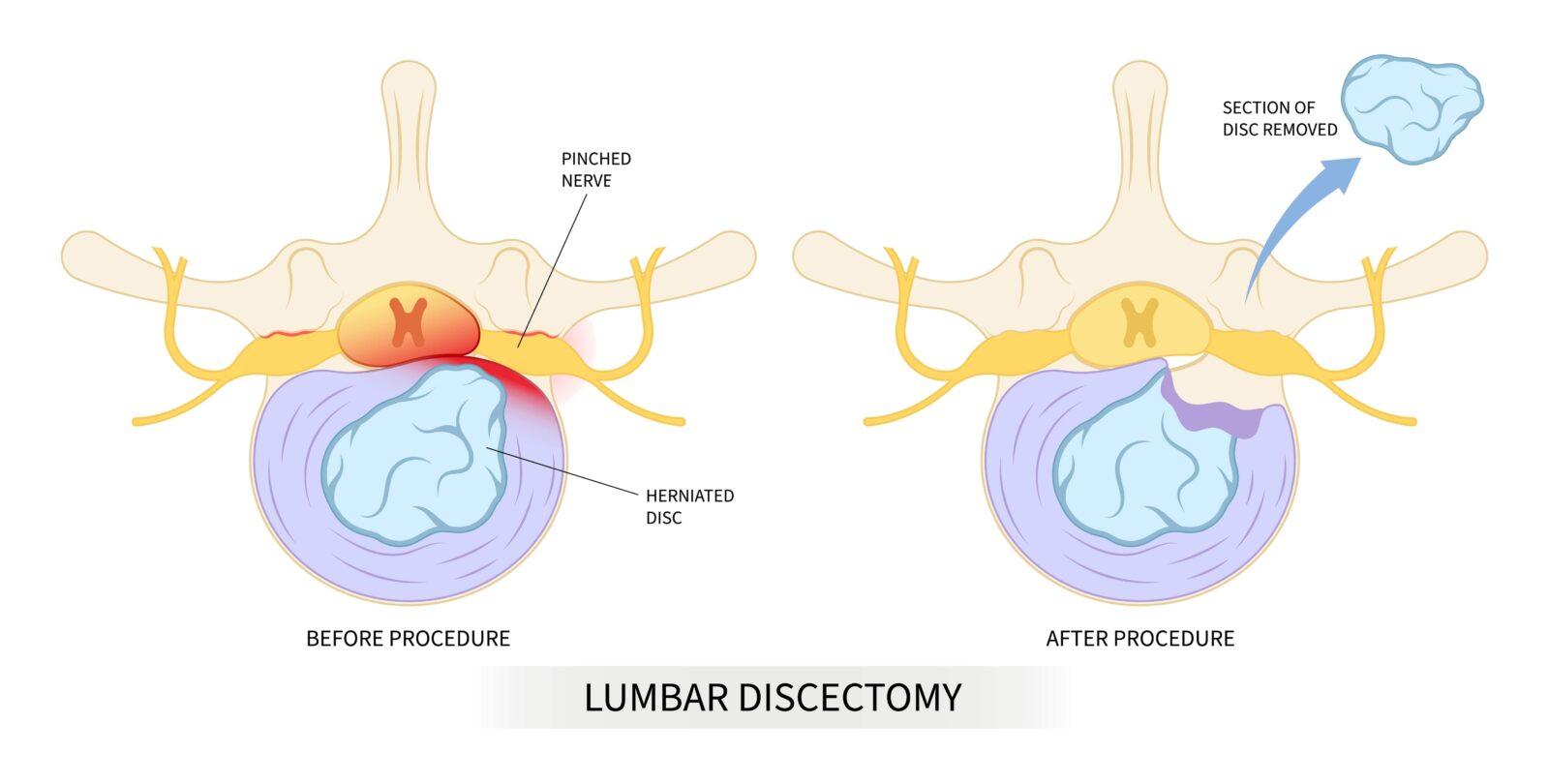
Surgery might be considered if the pain does not improve with non-surgical methods, or if there is significant weakness, loss of function, or severe pain due to nerve compression. Common surgical procedures include:
- Discectomy: Removal of the portion of the disc that is herniating and compressing a nerve root.
- Laminotomy or Laminectomy: Removing a small portion of bone over the nerve root, or removing the lamina (part of the vertebral arch) to relieve pressure.
- Spinal Fusion: Joining two or more vertebrae together to stabilize the spine after disc removal.
Alternative therapies:
Some patients find relief through alternative therapies such as chiropractic care, acupuncture, or massage therapy. These treatments may help some patients manage pain and improve function, particularly in combination with traditional medical treatments.
Treatment plans for herniated discs are highly individualized, based on the severity of the symptoms, the specific disc affected, and the patient’s overall health. Early treatment often improves the likelihood of a full recovery.
Conclusion
In conclusion, understanding herniated discs is vital for managing and potentially alleviating the painful symptoms associated with this condition. From recognizing the signs and causes to exploring various treatment options, each step is crucial in navigating the challenges of a herniated disc. Prevention strategies, such as maintaining a healthy weight, staying active, and practicing good posture, play an important role in protecting your spine health. If you suspect you may have a herniated disc, seeking professional medical advice promptly can lead to a more effective treatment plan and a better quality of life. Remember, while herniated discs can be a source of significant discomfort, with the right approach, many individuals find relief and return to their normal activities.