Minimally invasive spine surgery (MISS) represents a revolutionary approach in the field of spinal surgeries, aiming to reduce the trauma associated with traditional open surgeries. This technique has become increasingly popular due to its benefits like smaller incisions, reduced muscle damage, less pain postoperatively, and quicker recovery times. In this blog post, we’ll explore various types of spinal surgeries that can be performed using minimally invasive techniques.
Understanding Minimally-Invasive Spinal Surgery (MISS)
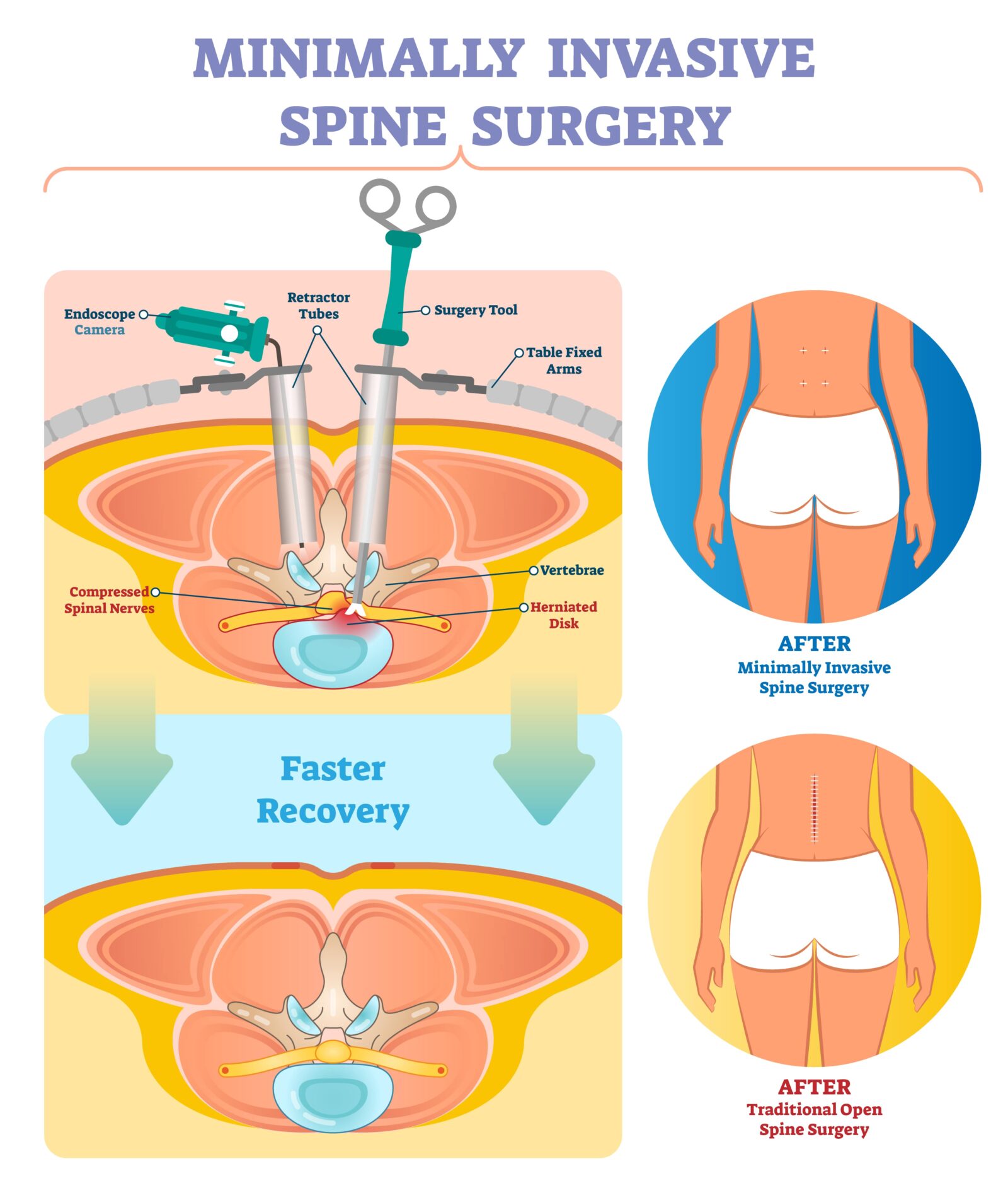
Minimally invasive spinal surgery (MISS) is a cutting-edge approach that stands in contrast to traditional open spinal surgeries. This innovative technique is characterized by its ability to reduce operative trauma, minimize postoperative pain, and accelerate patient recovery. At the heart of minimally invasive spinal surgery is the principle of minimizing tissue damage. Traditional spinal surgeries often involve long incisions through muscle and other tissues to access the spine. MISS, on the other hand, uses smaller incisions and specialized instruments. This approach significantly reduces the disruption of muscles and soft tissues surrounding the spine.
The advantages of minimally invasive spinal surgery are notable:
- Reduced Surgical Trauma: Smaller incisions mean less trauma to the body, which can lead to less pain and a quicker recovery.
- Lower Risk of Complications: The reduced disruption of tissues lowers the risk of surgical complications like infections and blood loss.
- Faster Recovery: Patients typically experience shorter hospital stays and a quicker return to daily activities.
- Less Postoperative Pain: Less tissue damage often translates into reduced postoperative pain, minimizing the need for pain medication.
Types of Surgeries That Can Be Performed Via MISS
The scope of minimally invasive spinal surgery is extensive, covering a range of procedures from lumbar decompression to spinal fusion and disc replacement. Each of these procedures is tailored to address specific spinal conditions, such as herniated discs, spinal stenosis, vertebral fractures, scoliosis, and more. Here are some spinal surgeries that can be performed using a minimally invasive technique:
Microdiscectomy
Microdiscectomy, a highly effective minimally invasive surgical procedure, is specifically designed to alleviate pain caused by herniated discs. In this procedure, the surgeon makes a small incision in the back, typically only about an inch long. Through this incision, using a microscope or magnifying instruments, the surgeon gains a detailed view of the affected area. The main goal of a microdiscectomy is to remove the portion of the intervertebral disc that is pressing on the nerve root, causing pain and other symptoms like numbness or weakness. To reach the herniated disc, a small amount of bone over the nerve root and/or disc material from under the nerve root is often removed. This direct approach allows the surgeon to decompress the nerve root carefully, thereby alleviating symptoms. The minimally invasive nature of this procedure means less damage to surrounding tissues, resulting in less postoperative pain and a quicker recovery time compared to traditional open back surgery. Microdiscectomy has become a preferred choice for many patients and surgeons alike due to its high success rate in relieving sciatic pain caused by disc herniation.
Laminectomy
A laminectomy, traditionally a major surgical procedure, can now be performed using minimally invasive techniques, significantly reducing the procedure’s impact on the patient. In a minimally invasive laminectomy, the surgeon makes a small incision in the back, often only a few centimeters long. Guided by advanced imaging techniques such as fluoroscopy, the surgeon inserts specialized instruments through this incision to reach the spine. The core objective of the surgery is to relieve pressure on the spinal cord or nerve roots, which is often caused by spinal stenosis – a narrowing of the spinal canal. The surgeon removes a small portion of the vertebral bone known as the lamina, along with any bone spurs or ligaments that are contributing to nerve compression. Unlike traditional open surgery, this minimally invasive approach avoids extensive muscle dissection and tissue trauma, leading to less postoperative pain, reduced risk of muscle damage, and a faster recovery period. This targeted, less invasive approach has made laminectomy a more feasible and less daunting option for many patients suffering from back pain and nerve compression symptoms.
Spinal Fusion
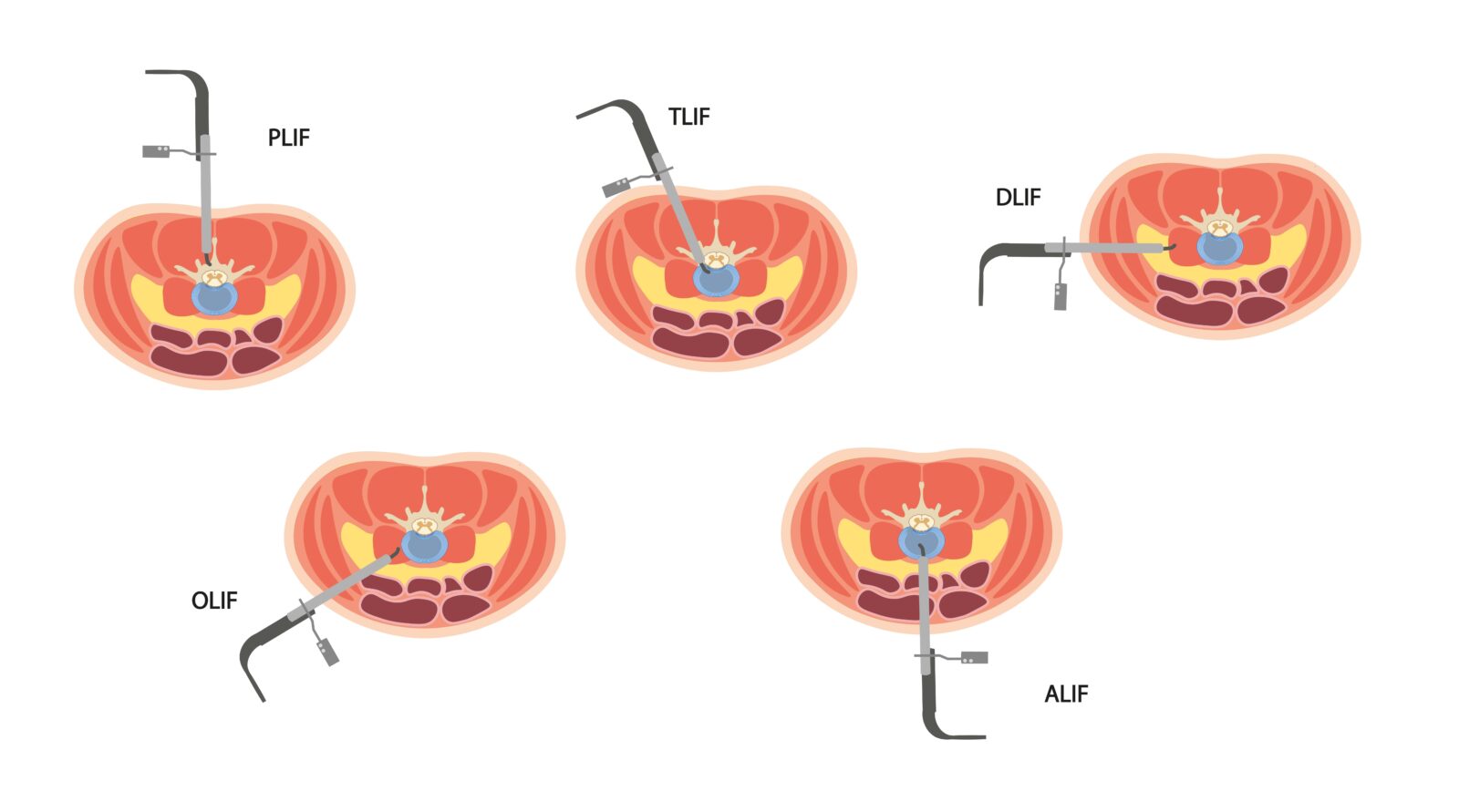
Spinal fusion, a procedure traditionally associated with significant tissue disruption, can now be performed using minimally invasive techniques, greatly enhancing patient recovery and outcomes. In minimally invasive spinal fusion, the surgeon makes small incisions in the back, significantly smaller than those in traditional open surgery. Through these incisions, specialized instruments and a guidance system are used to reach the affected vertebrae with minimal disruption to the surrounding muscles and tissues. The goal of spinal fusion is to permanently connect two or more vertebrae, providing stability to a damaged or unstable part of the spine. This is typically achieved by placing bone grafts or bone graft substitutes between the affected vertebrae. Rods and screws are then inserted to hold the vertebrae in place while the bone grafts fuse the vertebrae together over time. The minimally invasive approach reduces blood loss, lowers the risk of infection, minimizes muscle damage, and leads to a quicker recovery period compared to traditional spinal fusion surgery. This technique has become increasingly popular for treating conditions such as degenerative disc disease, spinal stenosis, scoliosis, or vertebral fractures, providing patients with a less invasive option with compelling benefits.
Foraminotomy
A foraminotomy, a surgical procedure aimed at relieving nerve compression in the spine, can be effectively performed using minimally invasive techniques, offering significant advantages over traditional open surgery. In this approach, the surgeon makes a small incision, typically only a few centimeters, near the affected area of the spine. Utilizing advanced imaging technology for precise guidance, the surgeon inserts specialized instruments through this incision to access the spine with minimal disruption to the surrounding tissues. The primary goal of a foraminotomy is to enlarge the vertebral foramen – the bony opening where nerve roots exit the spinal canal. This is achieved by carefully removing bone spurs, ligaments, or any other tissues that are compressing the nerves. The minimally invasive nature of this procedure significantly reduces tissue trauma, resulting in less postoperative pain, a reduced risk of complications, and a faster recovery time. This precise, targeted approach makes minimally invasive foraminotomy an increasingly preferred option for patients suffering from conditions like herniated discs, bone spurs, or spinal stenosis that result in nerve compression and associated pain or numbness.
Kyphoplasty and Vertebroplasty
Kyphoplasty and vertebroplasty are minimally invasive procedures designed to alleviate pain and stabilize the spine in patients with vertebral compression fractures, often due to conditions like osteoporosis. In both techniques, the surgeon makes a small incision in the back, just a few millimeters in length, through which a narrow tube is guided into the fractured vertebra under image guidance, typically using fluoroscopy. In vertebroplasty, this approach allows for the injection of a special bone cement directly into the collapsed vertebra, stabilizing the fracture. Kyphoplasty follows a similar procedure but includes an additional step before the cement injection. A small balloon is inserted and then gently inflated within the fractured vertebra. This inflation helps restore the height of the collapsed vertebra and creates a cavity that is subsequently filled with bone cement. Both procedures result in the stabilization of the vertebral fracture, offering significant pain relief and improved mobility. The minimally invasive nature of these techniques leads to reduced surgical trauma, lower risk of complications, and a quicker recovery compared to traditional open spine surgeries. These procedures provide a safe and effective treatment option for patients suffering from painful vertebral fractures.
Artificial Disc Replacement
Artificial disc replacement, a sophisticated alternative to spinal fusion, can be performed using minimally invasive techniques, offering a promising solution for patients with degenerative disc disease. In this approach, the surgeon makes a small incision, either on the patient’s abdomen or back, depending on the location of the affected disc. Utilizing advanced imaging techniques for precise navigation, the surgeon carefully moves aside muscles and soft tissues, creating a path to the spine with minimal disruption. The damaged disc is then meticulously removed and replaced with an artificial disc device. This artificial disc is designed to mimic the form and function of a natural spinal disc, preserving the spine’s mobility and flexibility. By avoiding a large, open incision, this minimally invasive approach significantly reduces tissue trauma, resulting in less postoperative pain, a reduced risk of complications, and a quicker return to normal activities. Artificial disc replacement through minimally invasive surgery represents a significant advancement in spinal care, providing patients with a viable option that maintains spinal motion and offers an enhanced quality of life post-surgery.
Conclusion
Minimally invasive spine surgery is a significant advancement in spinal care, offering patients effective treatment options with fewer complications and faster recovery times. However, it’s important to note that not every patient is a candidate for these procedures. A thorough evaluation by a spine specialist is necessary to determine the most appropriate treatment for individual conditions.